Hepatitis C Virus (HCV)
What sample is needed for the Hepatitis C Virus (HCV)?
- The best sample is the patient’s serum.
- The anti-HCV serum is stable for 7 days at room temperature.
- This test can also be done on the plasma.
- This test can be performed on a random sample.
What are the precautions for the Hepatitis C Virus (HCV)?
- Separate serum or plasma immediately to prevent viral degradation by white blood cells.
What are the indications for Hepatitis C Virus (HCV)?
- To diagnose the patient with HCV infection.
- For screening of the blood donor.
- This should be done to healthcare workers.
- Advised for the drug users.
- A person who has sex with a positive partner.
- In patients with HIV.
- In abnormal liver function tests.
- Blood transfusion or organ transplantation before July 1992.
- The patients with hemophilia were treated before 1987.
How will you define the Hepatitis C Virus (HCV)?
- This was formally called a non-A, non-B viral infection (NANB) because no tests were available. This was suspected by the exclusion of HBV and HAV.
- Hepatitis C is a blood-borne infection of the liver, and it leads to a high rate of chronic liver disease.
How will you discuss the history of viruses, NANB, or HCV?
- Later, the Hepatitis D virus was discovered and distinguished from NANB.
- NANB was also known as short-incubation and long-incubation viruses.
- The short-incubation virus was labeled as the Hepatitis E virus.
- The long-incubation name was still known as NANB.
- In 1991, the virus was identified as Hepatitis C Virus (HCV).
- The second-generation HCV test became available in 1993.
- A third-generation test for HCV was available in 1994.
- First and second-generation tests diagnose only HCV-IgG.
- HCV is the only virus with a long incubation period and was formerly known as the NANB virus.
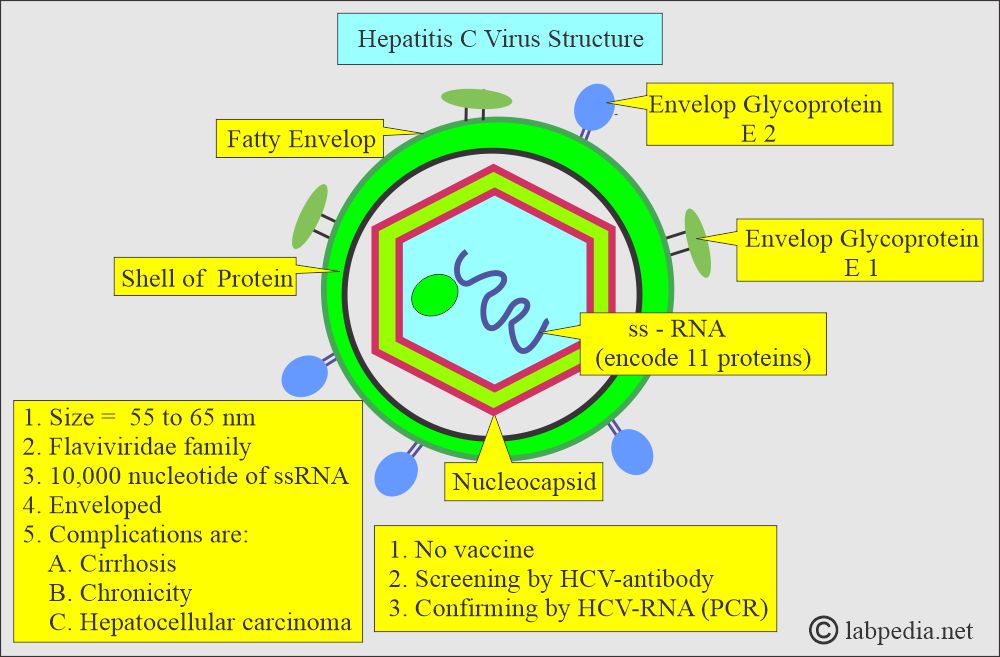
How will you discuss the biology and structure of the Hepatitis C Virus (HCV)?
- Hepatitis C virus (HCV) is a hepatotropic virus. It belongs to the Flavivirus family.
- HCV is a small enveloped virus measuring 55 to 65 nm.
- HCV is a small, positive-single-stranded RNA virus of the Flaviviridae family.
- HCV consists of 10,000 nucleotides of single-stranded RNA molecules in one common open reading frame.
- This was formally called a non-A, non-B viral infection because no test was available. This was suspected by the exclusion of HBV and HAV.
- HCV exists in 4 genotypes or strains:
- Core antigen.
- NS3 gene.
- NS4 antigen.
- NS5 antigen
- HCV infection differs from HBV infection in that it causes more than 60% of cases to become chronic.
- 20% of the patients develop cirrhosis and hepatocellular cancer.
What are the characteristic features of the Hepatitis C Virus (HCV)?
| Parameters | Characteristic features |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
What is the genetic variation of the Hepatitis C Virus (HCV)?
- HCV genotypes are detected based on treatment response.
- There are 6 genotypes with several subtypes.
- Genotype 1 progresses to chronicity and cirrhosis. It is less responsive to treatment.
- Genotypes 2 and 3 are very responsive to antiviral treatment.
- 75% of Americans have genotype 1, subtypes 1a and 1b.
- 20% to 25% have genotypes 2 and 3.
- Genotype 4 is more common in African countries.
- Genotype 5 is more common in South Africa and Asia.
- Genotype 6 is more common in Southeast Asia.
- The smaller percentage has genotypes 4, 5, and 6.
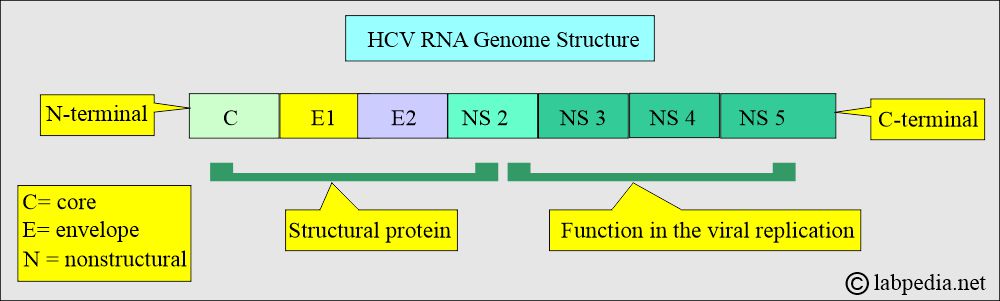
What is the Hepatitis C Virus (HCV) genome structure?
- It consists of an N-terminal and a C-terminal.
- There are core proteins, envelope proteins, and non-structural proteins.
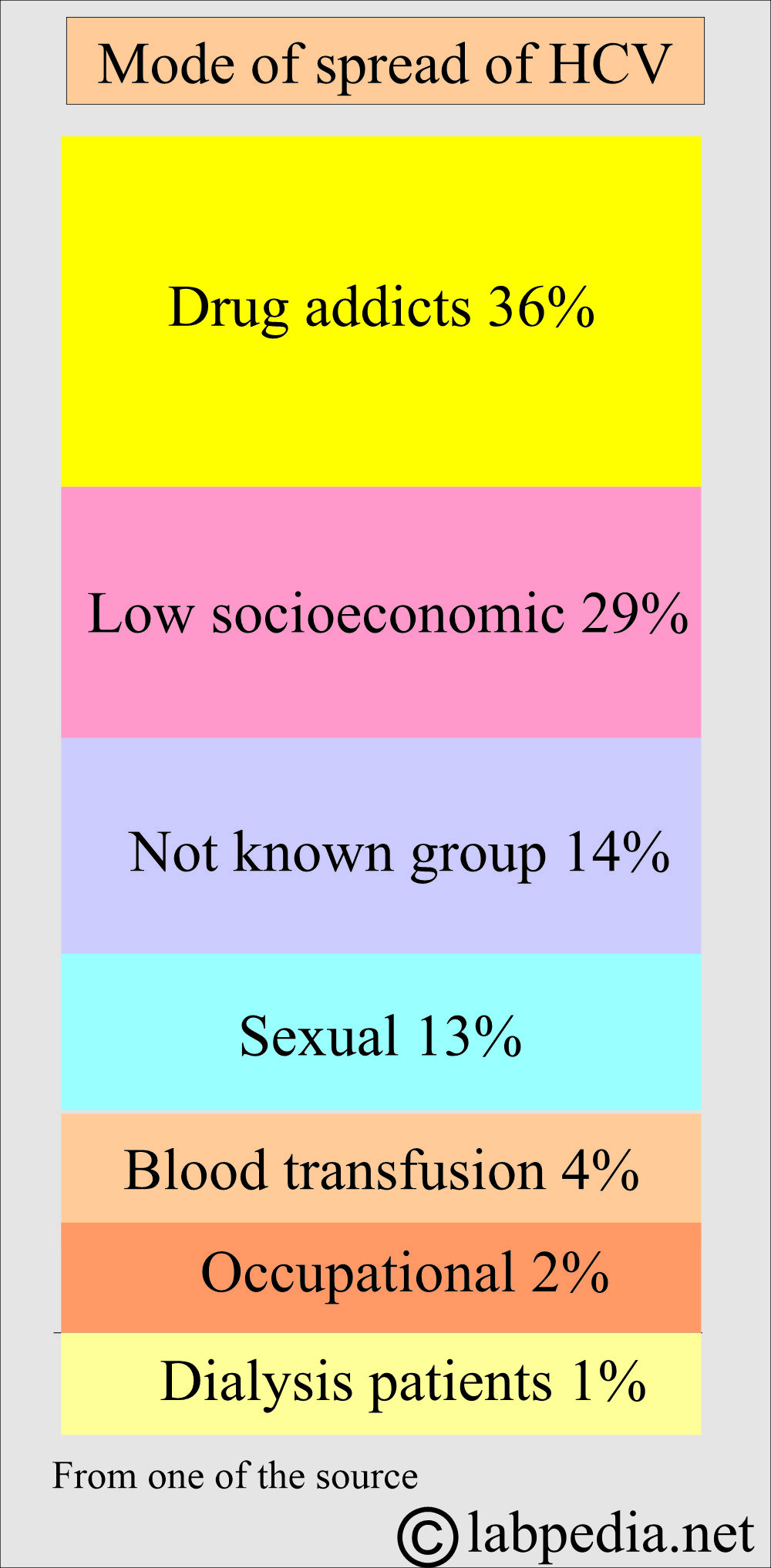
What is the mode of spread of the Hepatitis C Virus (HCV)?
- Blood (Serum).
- Saliva.
- Semen.
- Major risk groups are:
- Blood transfusion.
- I/V drug abusers.
- Blood products.
- The mode of spread is like HBV, with some differences.
- In 50% of cases, the source of the cases is unknown.
- One of the modes is blood transfusion or blood products (now rare because screening tests have been available since 1987).
- HCV hepatitis (post-transfusion hepatitis) is quite common in volunteer blood donors who are HBV-negative.
- Vertical transmission from mothers to newborns is not as common as HBV infection.
- This can spread through sexual contact, but some believe that sexual transmission is uncommon.
- This is seen in sex with multiple partners and unprotected sex.
- Male homosexuals are less likely to be infected as compared to HBV.
- It is also seen in smaller numbers in heterosexual groups.
- This is seen in organ transplantation (before 1992).
- This is common in I/V drug users.
- Tattooing in an unhygienic atmosphere.
- This may be seen in HIV patients.
- Sharing personal items, such as toothbrushes or shavers, that may be contaminated with blood.
- It is estimated that 50% of cases have an unknown mode of transmission.
- Fetal and neonatal transmission is uncommon.
- Passive transfer of anti-HCV antibodies is quite common.
What is the incubation period for the Hepatitis C Virus (HCV)?
- It is 2 to 12 weeks after exposure. (Other references give 2 to 52 weeks) and the average period is 7 or 8 weeks.
- Incubation of 2 weeks to one year is also reported.
What are the types of antigens and antibodies of the Hepatitis C virus (HCV)?
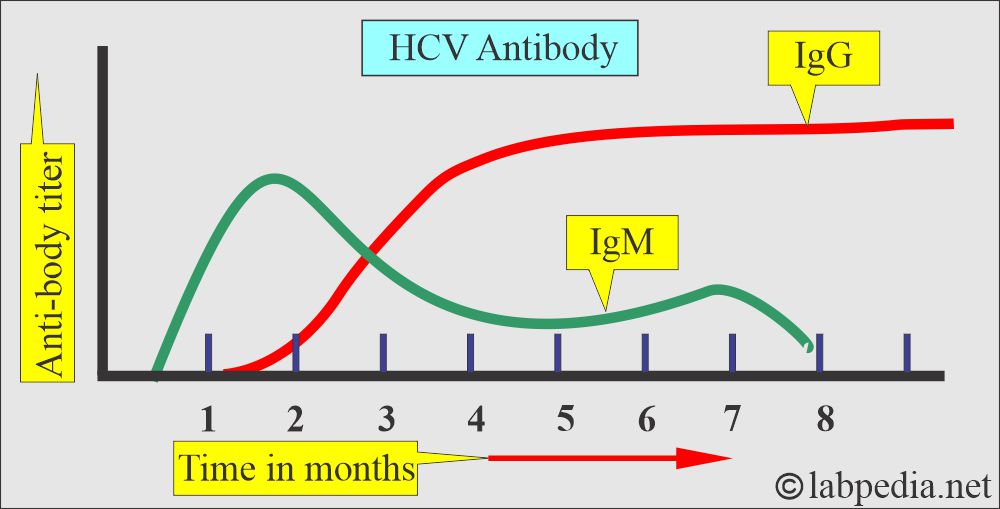
- HCV-Ab (IgG) appears in 3 to 4 months and disappears in 2 years.
- Most cases develop HCV-IgG antibodies by 6 weeks, with and range of 5 to 30 weeks after the onset of symptoms.
- The anti-HCV can be detected in acute hepatitis C during the initial phase of elevated aminotransferase activity.
- This antibody may never be detected in 5% to 10% of the patients with acute Hepatitis, and anti-HCV may become undetectable after the recovery from acute hepatitis.
- The current screening test detects antibodies against HCV.
- An anti-HCV screening test has been available for less than 10 years.
- This is a unique virus in which, during acute infection, you can detect anti-HCV antibodies and HCV RNA.
- Anti-HCV remains for many years. Therefore, a positive anti-HCV test indicates infection or carrier state but not infectivity or immunity.
What are the signs and Symptoms of the Hepatitis C Virus (HCV?
- HCV infection is also called a silent disease.
- The clinical S/S is like an HBV infection but less severe.
- It is in 12% to 25% of cases of sporadic hepatitis that are not related to parenteral inoculation or sexual transmission.
- Only 15% develop acute infection, and the rest develop chronic disease.
- Chronicity of the infection is seen in 50% to 80% of cases (another reference reports 70% to 80%).
- Chronicity is more common than HBV infection.
- It is seen in 60% of post-transfusion cases and may take 10 years.
- 30% of cases may develop cirrhosis in around 10 years.
- HCV infection may lead to chronic active hepatitis and cirrhosis.
- In one of the studies, chronic active hepatitis was seen in <20%, and 3% had cirrhosis.
- Fulminant hepatitis is seen in 1% to 2% of patients.
- HCV infection symptoms may not appear or may be very mild for years.
- Chronic infection is often asymptomatic.
- The silent disease still causes damage to the liver.
- The patient with the silent disease may come with chronic liver disease and may develop cirrhosis and liver cell carcinoma.
- It is considered a significant etiology for liver cell carcinoma.
What are the common symptoms of the Hepatitis C Virus (HCV)?
- Jaundice is seen in only 25% of acute hepatitis.
- Tiredness
- Loss of appetite
- Nausea and vomiting
- Abdominal pain
- Joints pain
- Fever
- Dark urine and gray-colored stool.
- Ultimately, the patient develops jaundice.
- This chronic viral infection can lead to liver cell carcinoma.
What is the Hepatitis C Virus (HCV) serological profile?
- An anti-HCV screening test has been available for less than 10 years.
- Anti-HCV Ab (IgG) indicates:
- Convalescent stage.
- Old HCV infection.
- Anti-HCV Ab (IgG) indicates:
- Anti-HCV antibodies are IgM and IgG types.
- Anti-HCV Ab seen against:
- Core antigen.
- NS3 gene.
- NS4 antigen.
- NS5 antigen.
- HCV PCR, which detects HCV RNA, is used to confirm the diagnosis.
- Viral load advises quantitative PCR.
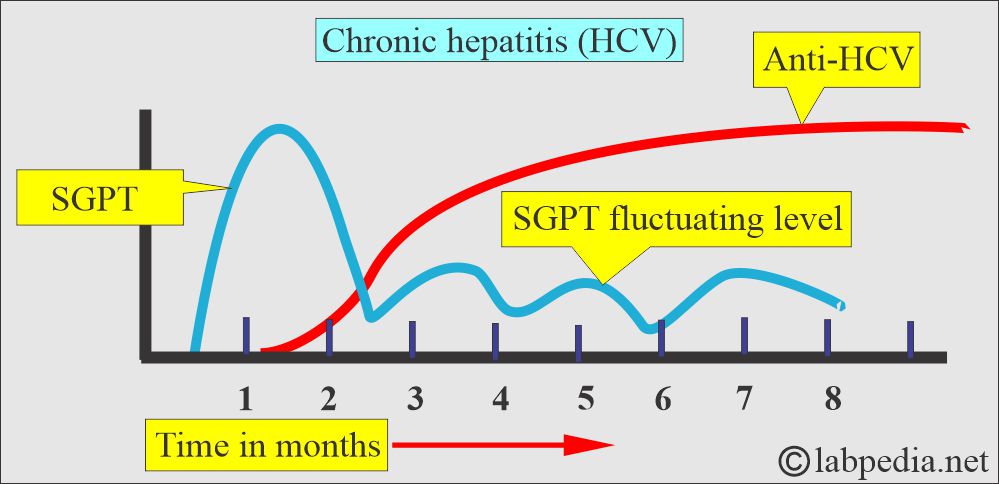
- Usually, SGPT (ALT) is raised in this infection and in chronic cases.
- A negative anti-HCV antibody test does not exclude HCV infection because seroconversion may not occur for up to 6 months after exposure.
How will you diagnose the Hepatitis C Virus (HCV)?
- Interpretation of HCV profile:
- Acute infection = Anti-HCV antibody will be positive.
- Anti-HCV by ELIZA is confirmatory.
- PCR can confirm the diagnosis.
- Qualitative PCR for the HCV genome.
- Quantitative HCV RNA PCR.
- PCR (polymerase chain reaction) will show the virus’s presence in the blood.
- PCR is the confirmatory test for HCV infection.
- PCR is performed in patients to initiate treatment.
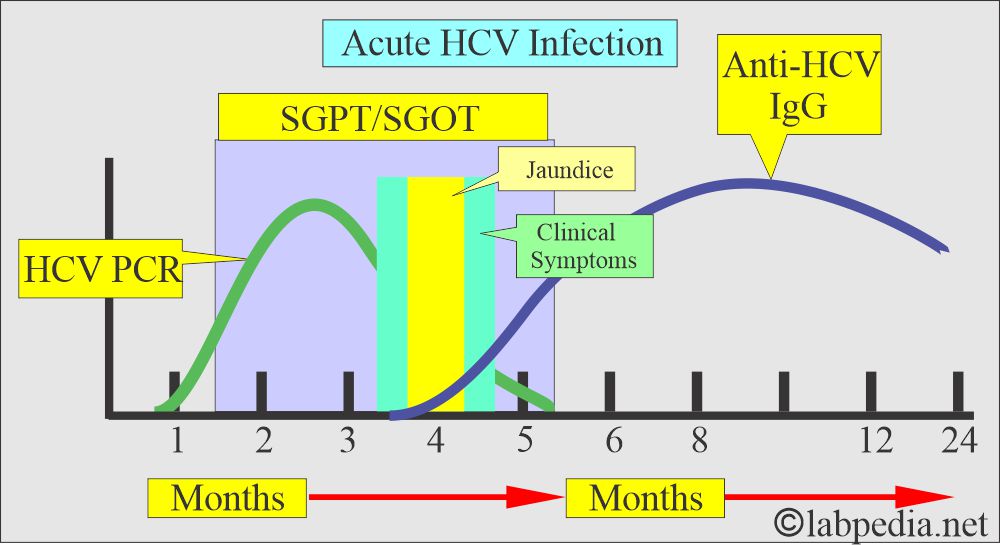
| Clinical features of Acute HCV infection |
|
| Laboratory workup |
|
Chronic infection: almost 85% show anti-HCV antibodies.
- Positive HCV-Ab indicates present or past infection.
| Clinical features of chronic HCV infection |
|
| Laboratory workup of chronic HCV infection |
|
What are the HCV markers in various diseases?
| Test | Normal | Early infection | Acute | Chronic | Carrier | Recovery |
|---|---|---|---|---|---|---|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
What is the interpretation of the HCV-antigen (HCV-Ag)?
- Nucleic acid probe without PCR:
- It appears about 3-4 weeks after infection.
- Nucleic acid probe with PCR:
- It becomes undetectable near the end of active infection, at the beginning of convalescence.
- RNA-PCR is positive after the second week of infection.
- It is undetectable after the end of active infection, beginning of the convalescent stage.
What is the interpretation of the HCV-antibody (HCV-IgG)?
- Done by ELIZA:
- It appears about 3-4 months after infection.
- 80% by 5 -6 weeks after the symptoms.
- It is undetectable in 7% of cases within 1.5 years.
- 7%-66% is negative by 4 years.
How will you summarize Hepatitis C Virus (HCV) antigen and antibody?
- HCV-antigen indicates acute infection.
- HCV-IgG indicates active, convalescent stage.
- It may also indicate an old infection.
What are the complications of Hepatitis C Virus (HCV) infection?
- There are chances for:
- Fulminant hepatitis is seen in 1% to 2% of patients.
- Cirrhosis is seen in 5% of cases.
- Liver failure.
- Liver cancer risk is 15%.
- HCV infection differs from HBV infection in that it causes more than 60% of cases to become chronic.
- (Some references say chronicity is from 50% to 80%)
How will you treat the Hepatitis C Virus (HCV)?
- Alfa-interferon alone. It benefits <50% of cases. Relapse is common when you stop the treatment.
- Interferon (IFN-α2, 3,000,000 U) is given subcutaneously 3 times per week for 1 year.
- It prevents the development of liver cell carcinoma.
- Monitor with SGPT, SGOT, and HCV PCR.
- Retreatment can be given in 50% to 80% of the relapse cases.
- Type 2 and 3 genotype-positive patients are three times more sensitive to antiviral treatments such as alpha-interferon or combination therapy with Ribavirin.
- Alfa-interferon with Ribavirin as combination therapy.
- The latest therapy can cure 95% of patients.
- To label the patient as cured, PCR HCV is negative for 3 months after completion of treatment.
How will you prevent the spread of the Hepatitis C Virus (HCV)?
- There is no vaccination available for HCV.
- Proper testing of blood donors for transfusion-related HCV has decreased the incidence.
How will you summarize the differences between HAV, HBV, and HCV viruses?
| Characteristic features | HAV | HBV | HCV |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Questions and answers:
Question 1: What is the chronicity in HCV infection as compared to HBV?
Question 2: Is there any possibility of a vaccine for HCV?

Here you say anti hcv last 2 years then you write many years. What is true?
Thanks for the question. I have elaborated on the statement in the text. Please see the link.
https://www.labpedia.net/hepatitis-c-virus-part-1-hcv-profile/