Growth Hormone (GH)
What sample is needed for Growth Hormone (GH)?
- This test is done on serum (clotted blood, 3 to 5 ml).
- A serum sample is preferred.
- Plasma (EDTA) has lower values with some methods.
- The patient should fast and rest for at least 30 minutes before taking the blood.
- It is stable for 8 hours at 2 to 8 °C.
- It can be kept for an extended period at -20 °C.
What are the precautions for Growth Hormone (GH) estimation?
- Perform the test immediately, as the half-life of GH is 20-25 minutes.
- Immediately refrigerate the serum.
- The patient should be fasting after midnight.
- The patient must fast and rest for 30 minutes before the sample is taken because this may increase the level.
- Avoid stress and low blood glucose, and exercise during the sample collection.
- EDTA plasma gives lower values.
- Random measurement is not helpful because of episodic variation in the GH level.
- Drugs that may increase the level are Amphetamine, Estrogen, Dopamine, Insulin, Methyldopa, Levodopa, Histamine, and Nicotinic acid.
- Certain drugs that decrease GH levels are Phenothiazine and Corticosteroids.
What are the indications for Growth Hormone (GH)?
- Growth hormone (GH) is used to identify its deficiency in:
- Adults with short stature.
- Delayed sexual maturity.
- Or other growth abnormalities.
- To diagnose gigantism or acromegaly,
- This can be used to identify the pituitary hypofunction or hyperfunction.
How will you define Growth Hormone (GH) and its structure?
- Growth hormone (GH) is a peptide secreted by the pituitary gland’s acidophilic cells.
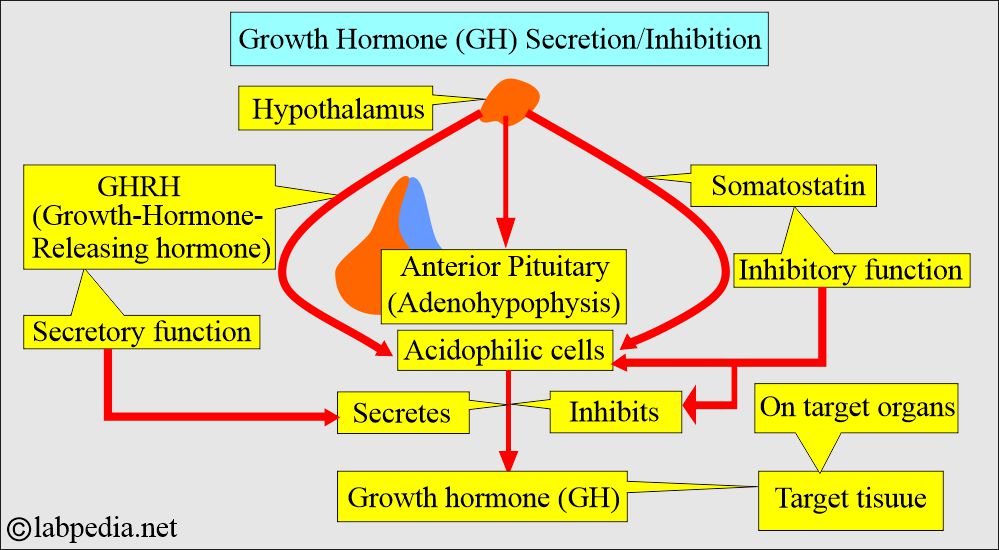
- GH is produced and secreted by somatotropes in response to the hypothalamic secretion of growth hormone-releasing hormone (GHRH) and is inhibited by somatostatin.
- GH is also called somatotropin.
- Hypothalamus hormones:
- Growth hormone-releasing hormone (GHRH) stimulates Growth hormone (GH) release.
- Somatostatin inhibits the release of Growth hormone (GH).
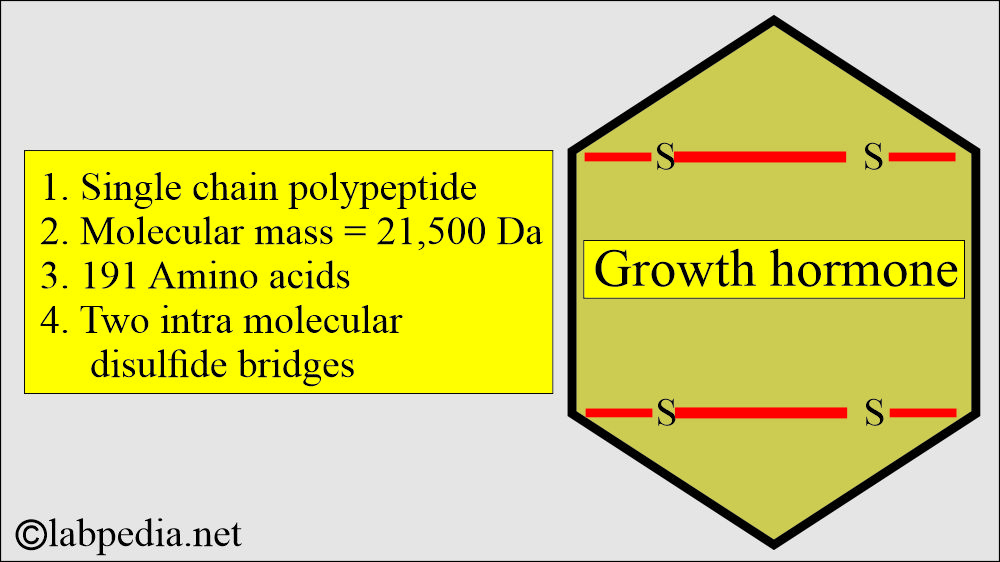
- The growth hormone is a single-chain polypeptide with a molecular weight of 21,500 Da (22 kDa) and 191 amino acids.
- It has two intramolecular disulfide bridges.
- Its structure is similar to prolactin.
- This is one of the hormones involved in growth produced by the pituitary gland.
- Somatotropin is a man-made hormone.
- It is stored in the cells as intracellular granules.
- Growth hormone production is pulsatile.
How will you discuss the pathophysiology of growth hormone (GH)?
- Growth hormone (GH) plays a role in growth from birth until the end of puberty.
- GH promotes protein synthesis and stimulates skeletal growth.
- Various factors increase Growth hormone (GH) secretion.
- Growth hormone (GH) is produced by the anterior pituitary gland’s acidophilic cells and stored within the intracellular granules.
- Growth hormone (GH) secretion occurs predominantly during sleep in irregular pulses or bursts.
What are the types of adenohypophysis (anterior Pituitary gland) hormones?
| Hormones | Type of the cells | Shortcut names |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
What is the difference between the pituitary gland and the adenohypophysis?
| Features | Pituitary gland | Adenohypophysis |
|
|
|
|
It consists of:
|
|
|
|
|
The pituitary gland is involved in the regulation of:
- Growth.
- Development.
- Adrenal function.
- Thyroid function.
- Gonadal function.
- Water and salt homeostasis.
How will Growth Hormone secretion be?
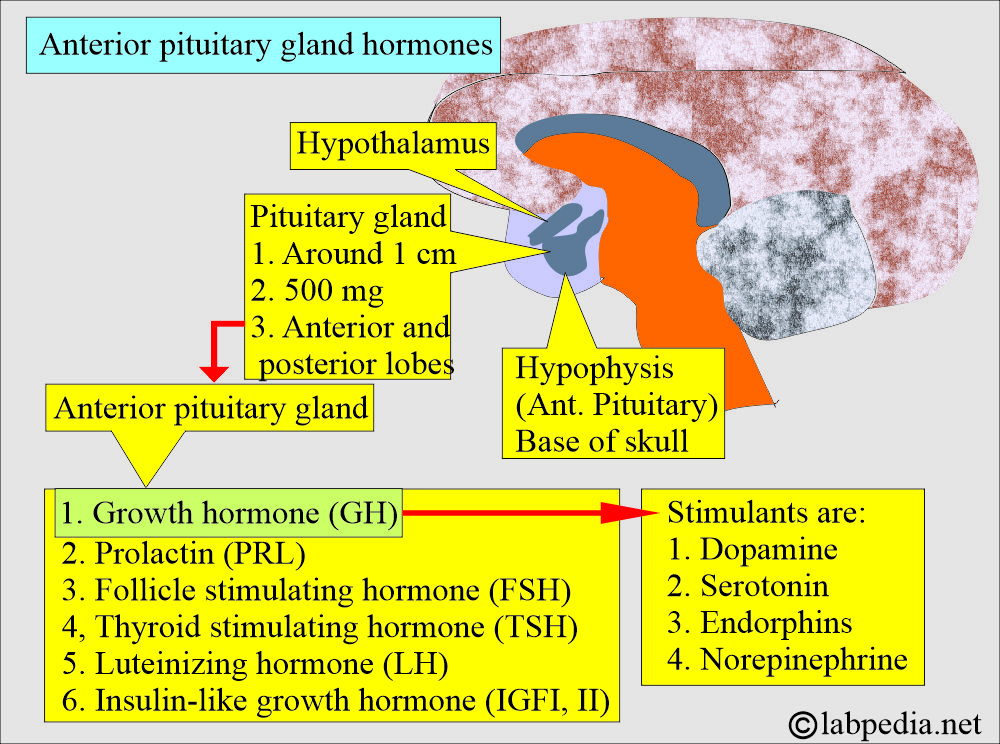
- Anterior pituitary gland (acidophilic cells secrete):
- Growth hormone.
- Prolactin.
- Thyroid-stimulating hormone (TSH).
- Follicle-stimulating hormone (FSH).
- Luteinizing hormone (LH).
- Insulin-like growth factor.
- Hypoglycemia stimulates the pituitary gland to secrete GH.
- It is an antagonist to insulin.
- This was used as a stimulation test, but it was not safe.
- Arginine stimulates GH secretion.
- Growth hormone (GH) increases glucose by:
- Inhibiting the entry of glucose into the muscle cells.
- By inhibiting glycolysis.
- By inhibiting the formation of triglycerides from glucose.
What is the Growth hormone (GH) controlling mechanism?
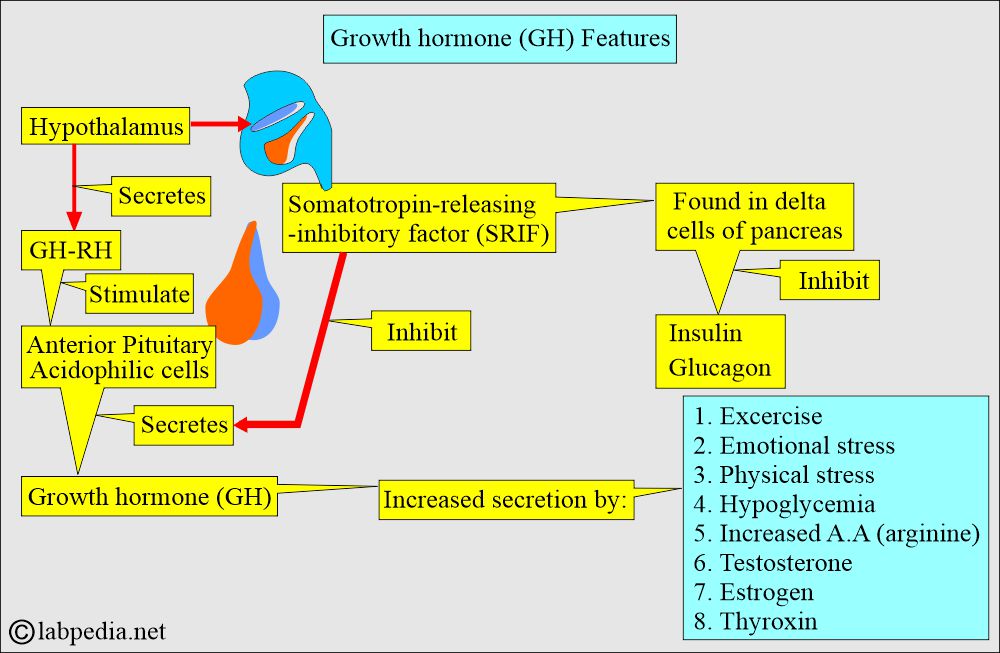
- Two hypothalamic factors secreted into the portal circulation from nerve terminals in the median eminence control growth hormone (GH) release.
- Growth hormone-releasing hormone (GH-RH) stimulates GH release into the circulation.
- Somatotropin release-inhibitory factor (SRIF) will inhibit the GH release into the circulation.
- SRIF is found in pancreatic islet delta cells and other sites in the digestive tract.
- SRIF also has another important function: inhibiting the release of insulin and glucagon.
- Growth hormone (GH) affects many tissues through a group of peptides (Somatomedins).
- Increased levels of Somatomedins lead to increased production of Somatostatin, which is released from the hypothalamus.
What are the variations in Growth hormone (GH) production?
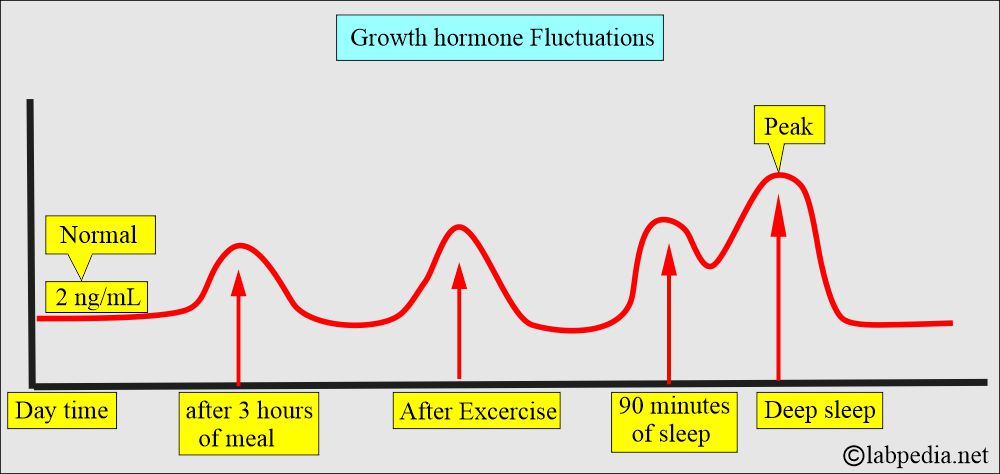
- GH has a diurnal variation in concentration.
- Stimuli leading to an increase in Growth hormone (GH):
- Exercise.
- Physical and emotional stress.
- Ingestion of protein.
- In hypoglycemia.
- Spike occurs after 3 hours of meals or exercise.
- The level is low during the day and is around 5 ng/mL (another reference says <2 ng/mL).
- For adults and children in the evening, it is the highest level.
- GH secretion is episodic and variable; the level may reach 40 ng/ml in a healthy subject.
- The highest values are noted during the deepest sleep level. So its level is increased during sleep.
- So the best time is 60 to 90 minutes after a deep sleep.
- Or do the exercise for 30 minutes and get the GH sample, which will be at the highest level.
- The GH may increase ten times the normal level during sleep.
- GH test may be used to monitor the acromegaly treatment.
- Obesity reduces GH release and the insulin response.
- Hypoglycemia stimulates the pituitary to secrete GH.
- The ability to secrete GH in response to conventional challenges decreases with age.
- GH is tested in case of retarded growth or short stature.
What are the stimuli for the growth hormone (GH) secretion?
| The stimulus for the secretion of Growth hormone (GH) | Time of peak level of Growth hormone (GH) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
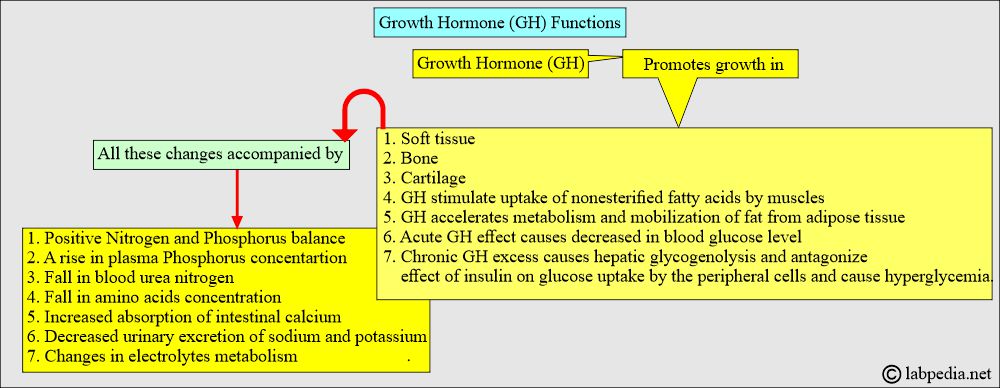
What are the functions of the growth hormone (GH)?
- GH in insufficient amounts leads to:
- Limited growth.
- Its deficiency leads to dwarfism.
- Delay in maturity.
- GH overproduction leads to :
- Its excess leads to gigantism.
- Acromegaly. (Increase in bone thickness and width).
- It promotes protein synthesis in muscles.
- It promotes protein synthesis in the liver.
- It stimulates skeletal muscle growth.
- It directly stimulates amino acid uptake.
- GH is important for anabolic and repair functions and proper skeletal growth.
- GH has an anti-insulin effect on carbohydrate metabolism.
- In fasting, insulin secretion decreases, and GH secretion increases, stimulating the body to use fatty acids instead of glucose.
What is the Clinical presentation of growth hormone (GH) excess?
- Excess GH is seen in the eosinophilic or chromophobe adenomas of the pituitary gland.
- 75% of these tumors can be diagnosed on CT scans or MRIs.
- Prolonged exposure to GH leads to overgrowth of the skeleton, muscles, and soft tissues.
- It is usually seen in adults and is called Acromegaly.
- This condition is called Pituitary gigantism, when excess GH is seen before long bone growth is complete.
What are the various types of growth hormone (GH) tests?
- A growth stimulation test can be done to evaluate the deficiency.
- An exercise stimulation test can be advised for GH.
- Brisk exercise increases GH.
- This test can be done in the morning after an overnight fast or at any time.
- The patient is advised to exercise vigorously for 20 minutes.
- Collect blood immediately after exercise terminates.
- If GH is >7 ng/ml, it is less likely to be due to a deficiency.
- 3 to 6 ng/mL is an intermediate response, considered a suspected case.
- The growth suppression test is performed in adults with gigantism and acromegaly.
- An oral glucose tolerance test is very helpful for determining glucose levels. Normally, GH is suppressed. However, in acromegalic patients, there is a slight or no decrease in GH.
- Give 75 to 100 grams of glucose over 5 minutes, then collect a GH sample at 30, 60, 90, and 120 minutes.
- In an insulin-induced hypoglycemia stimulation test:
- Hypoglycemia triggers the release of GH and ACTH from the pituitary glands in a normal person.
- Give I/V insulin to overnight fasting patients.
- Insulin 0.1 to 0.15 U/Kg body weight is injected I/V.
- Collect the blood sample after a 30-minute rest period for GH, ACTH, and cortisol.
- Collect blood samples at 30, 60, and 90-minute intervals.
- Estimate glucose, GH, ACTH, and cortisol.
- The patients may become symptomatic and develop hypoglycemia <40 mg/dL.
- This test is contraindicated in patients with seizures and ischemic heart disease.
- GH level reaches >10 ng/mL.
- Cortisol level reaches a peak value of >20 µg/dL.
- Direct Measurement of Growth hormone (GH) can be performed by bioassay, receptor assay, and immunoassay.
Acromegaly:
How will you define acromegaly?
- Acromegaly in adults is caused by increased growth hormone (GH) secretion.
- The most common cause may be the eosinophilic adenoma of the pituitary gland.
- Roughly 2/3 of the patients are female.
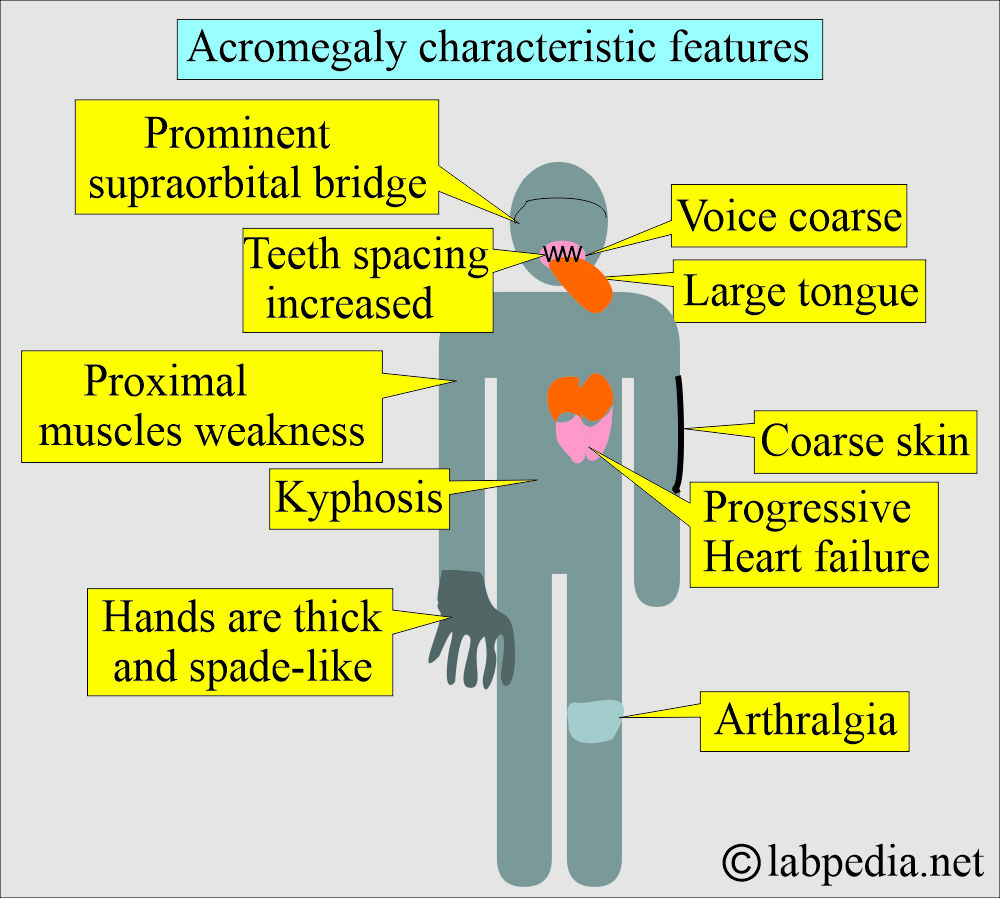
How will the clinical presentation of the acromegaly be?
- The excess of GH leads to Acromegaly.
- Pituitary gigantism is seen before the long bone growth is complete.
- The patient’s physical appearance can help diagnose this.
- There is an overgrowth of soft tissue and bone.
- There is coarse, oily skin.
- There is a large tongue.
- There are prominent supraorbital ridges.
- The spacing between teeth is increased.
- Hands are thick, spade-like.
- The patient will have arthralgia and kyphosis.
- The voice is coarse.
- The patient may develop proximal muscle weakness.
- Sweating and headaches are common.
- The patient will have progressive heart failure.
- The reversibility of the physical changes depends upon the duration of the disease.
- Acromegaly may lead to severe disability or death due to cardiac or neurological complications.
- There is an abnormal GH response to oral glucose administration.
- A normal person shows <1 ng/mL of GH after an oral dose of glucose.
What are the Complications of Acromegaly?
- The patient may develop diabetes mellitus.
- The patient will have hypertension and cardiomegaly.
- There is obstructive sleep apnea.
How will you diagnose Acromegaly?
- The diagnosis of acromegaly depends on elevated growth hormone (GH) levels.
- Advise the glucose tolerance test:
- Collect a blood sample at 0, 30, 60, and 90 minutes.
- Estimate both glucose and GH.
- The values will be suppressed at around <1.0 ng/mL.
- Another test is IGF-1 (insulin-like growth factor-1), whose concentration increases in acromegaly.
How will you treat the Acromegaly?
- Acromegaly due to an adenoma is treated with a transsphenoidal resection of the tumor.
- Another method is gamma knife multiport irradiation.
- Somatostatin (SST) long-acting needs only one dose per month.
What will be the presentation of the deficiency of growth hormone?
- This is usually seen in hypothalamic and pituitary tumors.
- Growth is a sign of dwarfism and short stature in the child.
How will you diagnose growth hormone (GH) deficiency?
- Advice: Two stimulating tests, such as insulin hypoglycemia or arginine.
- Measure GH at 30, 60, and 90 minutes.
- Normal patients show an increase in GH to >8.0 ng/mL.
What is normal growth hormone (GH)?
Source 1
| Age | ng/mL |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
- To convert into SI units x 1.0 = µg/L
Source 2
|
|
|
|
|
|
|
|
- The random GH level provides little diagnostic information.
- A single estimate may not be helpful due to variation in GH levels throughout the day.
What are the causes of increased Growth hormone (GH)?
- Pituitary gigantism (Acromegaly = up to 400 ng/ml).
- Ectopic GH secretion, e.g., Stomach neoplasm, lung.
- Renal failure.
- Cirrhosis.
- Stress, exercise, prolonged fasting.
- Uncontrolled diabetes mellitus.
- Anorexia nervosa.
- Starvation and malnutrition.
- Hypoglycemia.
- Major surgery.
- Exercise.
What are the causes of decreased growth hormone (GH)?
- Pituitary dwarfism, hypopituitarism.
- Adrenocortical hyperfunction.
- Hyperglycemia.
- Delayed sexual maturity.
- Growth hormone deficiency.
Questions and answers:
Question 1: When is the peak level of GH?
Question 2: What are the complications of acromegaly?