Cryoglobulins Classification and Diagnosis
Cryoglobulins
What Sample is needed for cryoglobulins?
- Venous blood is needed. Collect 10 mL of the venous blood in red-top tubes that are prewarmed to body temperature.
- Keep the blood at 37 °C.
- Separate the serum at 37 °C so the cryoglobulins remain in the serum.
What are the Precautions for detecting cryoglobulins?
- Maintain the temperature of the blood at 37 °C.
- Also, maintain the temperature of the serum at 37 °C.
What are the Indications for detecting the cryoglobulins?
- This test is done to diagnose:
- Purpura.
- Arthralgia.
- Raynaud phenomenon.
What is the definition of Cryoglobulins?
- These abnormal immunoglobulins precipitate in serum reversibly at low temperatures or may gel at cold temperatures.
- Most cryoglobulins are polyclonal immunoglobulin complexes, and nearly half are monoclonal, usually IgM.
- Cryoglobulins are abnormal immunoglobulin proteins produced due to various diseases.
- Cryoglobulins reversibly precipitate at low temperatures and redissolve with rewarming.
What are the Cryoglobulins’ properties?
- These are insoluble at 4 °C.
- May aggregate up to 30 °C.
- It can fix a complement.
- It can initiate an inflammatory response.
| Properties of cryoglobulin | Clinical description |
|
|
|
|
|
|
|
|
|
|
|
May cause vasculitis due to:
|
|
|
|
|
How will you define Cryoglobulinemia?
- It is defined as a condition where plasma or serum proteins (IgM) precipitate when cooled below body temperature.
- These proteins precipitate at 4 °C and dissolve again at 37 °C.
- These are the proteins that reversibly precipitate or gel at 4 °C.
How will you classify Cryoglobulins?
- Type I (Monoclonal).
- Type II (Mixed cryoglobulin, a mixture of polyclonal immunoglobulins).
- Type III (Polyclonal).
- What are the causes of Cryoglobulinemia?
- Primary, idiopathic, or essential.
- Secondary that is associated with diseases.
What are Type I (monoclonal) cryoglobulins?
- These are produced by the neoplastic lymphocytes and plasma cells. These are typically IgM types of immunoglobulin.
- Associated with multiple myeloma, macroglobulinemia, and rare neoplasms of the plasma cells and lymphocytes.
- Blood may gel when drawn.
- Sometimes, these are idiopathic.
- May see IgG as well.
- Rarely see IgA only.
- These may constitute 25% of the cryoglobulins.
- Often present in large amounts >5 mg/dL in the serum.
- Symptoms are severe, and often, there may be gangrene without any other cause.
- The patient may have Raynaud’s syndrome-like symptoms.
What are Type II cryoglobulins?
- These are monoclonal immunoglobulins mixed with one type of polyclonal immunoglobulin; the most common is IgM, and polyclonal IgG, always seen with RF.
- It is seen in 25% of the cases.
- The Type II cryoglobulins consist of two types:
- The monoclonal form is seen as the rheumatoid factor and usually is IgM with a light kappa chain.
- The second is polyclonal IgG, which is always seen as a Rheumatoid factor (RF).
- RF may be seen as a high titer without the disease.
- It is most often seen with HCV infection and less frequently with HBV, EBV, and other diseases like bacterial infection, parasitic infestation, autoimmune disorders, Sjogren’s syndrome, and immune complex nephritis.
- The C4 level is decreased.
What are Type III cryoglobulins?
- These are mixed cryoglobulins and the most common combination of IgG and IgM (usually with RF).
- It is seen in ∼50% of the cases.
- It usually occurs in a small amount of <1 mg/dL in the serum.
- More than 90% contain IgM, rheumatoid factor, and IgG.
- It is most commonly seen with lymphoproliferative disorders and connective tissue diseases like SLE.
- These are also seen in patients with persistent HCV infection.
- Mostly seen in autoimmune diseases.
- Various antigens, such as viral, bacterial, and autologous antigens, produce circulating immune complexes.
What is Mixed cryoglobulinemia?
- It consists of type II and type III.
What are the Causes of Cryoglobulins?
- Autoimmune diseases like SLE, RA, and Sjogren’s syndrome.
- Malignancies like Multiple myeloma, Leukemia, Waldenstrom macroglobulinemia, and Lymphoma.
- Acute and chronic infections like Infectious mononucleosis, Poststreptococcal glomerulonephritis, and endocarditis.
- Liver diseases like Cirrhosis and Hepatitis.
- Renal involvement manifests as either nephrotic or nephritic syndrome associated with hypocomplementemia.
- The most common finding is membranoproliferative glomerulonephritis type II.
What are the Signs and Symptoms of Cryoglobulins?
- Cryoglobulinemia is a systemic immune-complex disease characterized by a clinical syndrome:
- Palpable purpura. This is a constant feature and is present in the lower extremities.
- Arthralgias.
- Hepatosplenomegaly.
- Lymphadenopathy.
- Anemia.
- Glomerulonephritis. The most common is membranoproliferative glomerulonephritis ( MPGN type II).
- Most patients are hypocomplementemic, reflecting immune-complex disease.
- These proteins precipitate in the blood vessels of fingers when exposed to cold.
- These patients will have symptoms of:
- Vascular purpura. This is the most common symptom and is seen in 60% to 100% of the patients.
- Bleeding tendency.
- Arthralgia. It is the second most common, seen in 60% to 90% of the cases.
- Cold-induced urticaria.
- Raynaud phenomenon (pain, cyanosis, the coldness of fingers). It is seen in 50% of the cases.
- These proteins are present in various diseases.
- Serum level >5 mg/dL = Multiple myeloma, macroglobulinemia, and leukemia.
- Serum level between 1 to 5 mg/dL= Rheumatoid arthritis.
- Serum level <1 mg/dL = SLE, RA, infectious mononucleosis, viral hepatitis, endocarditis, cirrhosis, glomerulonephritis.
| Type of cryoglobulin | Type of Immunoglobulins | Diseases |
|---|---|---|
|
|
|
|
|
|
|
|
|
What are Normal Cryoglobulins?
- The serum is negative for cryoglobulins.
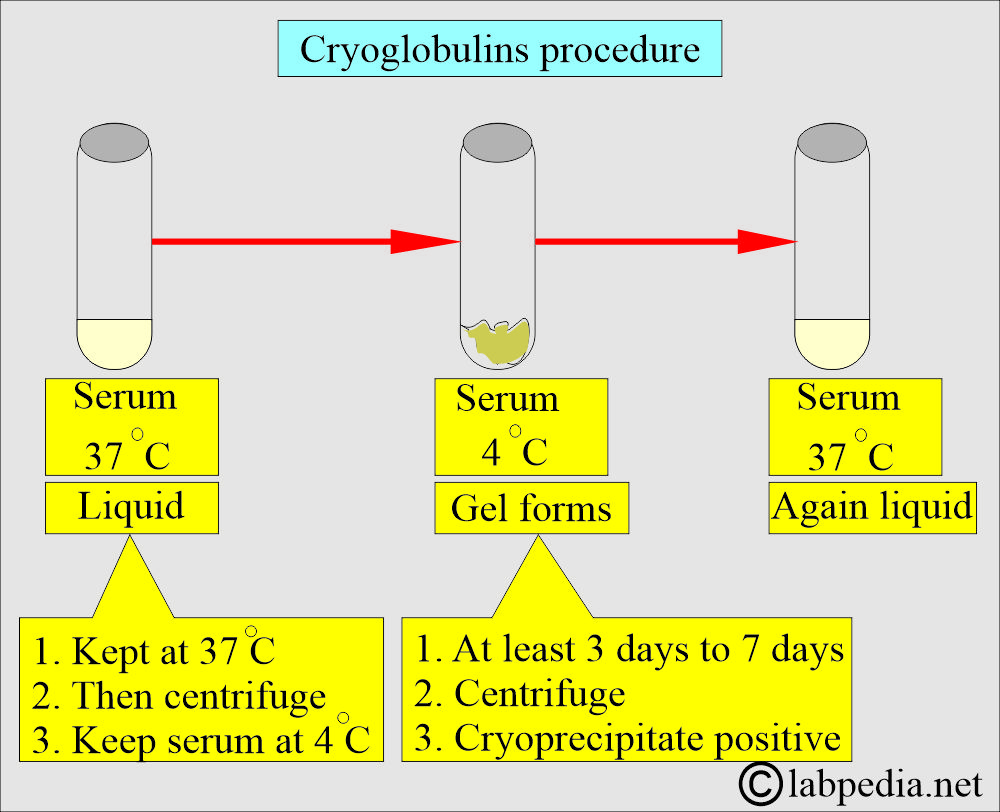
What is the Procedure for Cryoglobulins?
- Take the blood and keep it at 37 °C until it is clotted.
- Clotted blood is centrifuged at 37 °C.
- Keep the serum in the fridge at 4 °C.
- Please keep it for at least 3 days and again centrifuge at 4 °C.
- Check the serum daily for white precipitate or gel.
- Checking the time period is disputed; some suggest 3 days, while others propose 7 days.
- Check daily for at least 72 hours to 7 days.
- The precipitate recorded and measured is cryoglobulin.
- Rewarm the sample if it dissolves, then it confirms the cryoglobulins.
- Cryoprecipitate is washed and subject to Immunoelectrophoresis to identify the type of cryoglobulin (immunoglobulin).
What is another procedure for cryoglobulin?
- Collect the blood in EDTA or citrate, and also make a serum sample.
- Incubate both at 4 °C.
- A precipitate in the plasma but not in the serum will indicate cryoglobulins.
How will you differentiate cryoglobulins and cold agglutinins?
| Parameters | Cryoglobulins | Cold agglutinins |
|
These are immunoglobulins. | These are autoantibodies like IgM. |
|
Precipitate in cold (4 °C)and dissolve again at a warm temperature (37 °C) | These will agglutinate RBCs at cold temperatures |
|
Soluble in plasma and forms immune complexes | RBCs surface antigens |
|
Precipitate at 4 °C and redissolve at 37 °C | Agglutinate RBCs at 4 °C to 30 °C |
|
Maybe IgM, IgG, or IgA, or mixed | Mostly IgM and rarely IgG |
|
|
|
|
No direct effect except in vasculitis | Hemolysis due to activation of the complement |
|
|
|
|
|
|
|
|
Perform direct agglutination using RBCs and the patient’s serum at a cold temperature. |
|
|
|
How will you treat cryoglobulins?
- Immune modulation is attempted using corticosteroids, especially in mixed types of cryoglobulins.
- Can try plasmapheresis.
- α-interferon in patients with HCV.
- Remissions are achieved in 75% of the cases of mixed type.
- Relapse is seen in 50% of the cases in mixed type.
Questions and answers:
Question 1: What are type 1 cryoglobulins?
Question 2: What is the definition of cryoglobulinemia?