Red Blood Cell (RBC):- Part 4 – Red Blood cell Indices Interpretations
Red Blood Cell Indices Interpretations
What blood sample is needed for Red Blood cell Indices?
- For Blood indices, the best sample is EDTA blood.
- Collect the blood in the lavender top tubes.
- Transport the blood to the lab and run in the hematology analyzer to calculate blood indices.
- Blood is stable for 6 hours at 25 °C and for 24 hours at 4 °C.
- Fetal blood is collected percutaneously from the umbilical area.
What are the indications for Red Blood cell Indices?
- These tests help diagnose various types of anemia.
What are the precautions for Red Blood Cell Indices?
- The abnormal size of RBC may affect indices.
- An increased count of WBC will affect the indices.
- Increased reticulocyte count leads to abnormally high MCV.
- Cold agglutinins give false increased values of MCH, MCHC, and MCV.
What is the definition of Red Blood cell Indices?
- Red cell indices define the size and contents of hemoglobin in Red blood cells.
Mean corpuscular volume (MCV):
How will you define MCV?
- This is the average volume of red blood cells measured in cubic micrometers (µ3, femtoliter fL).
- This indicates the cell size of RBCs.
- This is the best index for classifying anemia.
What are the indications of MCV?
- It helps in the classification and differential diagnosis of anemia.
- It is a helpful screening test for occult alcoholism.
What are the factors interfering with MCV?
- In the case of leucocytosis, there is increased MCV.
- Marked hyperglycemia increases MCV.
- Cold antibodies increase MCV.
- Methanol poisoning increases MCV.
- In the case of increased reticulocytes, there is increased MCV.
- Hemolysis leads to a decrease in MCV.
How will you calculate MCV?
- MCV is calculated by dividing hematocrit by the total RBC count.
What is the normal MCV?
- Adult (all ages) = 80 to 95 fL
- Newborn = 96 to 108 fL
How are RBCs classified based on MCV?
- Macrocytes are present when the MCV value is high, e.g., in megaloblastic anemia due to vitamin B and folic acid deficiency.
- In macrocytic anemia, MCV is 100 to 150 fL (>100 fL).
- Microcytes, when the MCV is decreased, are seen in iron deficiency anemia and thalassemia.
- In microcytic anemia, MCV is 50 to 82 fL.
- Normochromic normocytic anemia, MCV is 82 to 98 fL.
- Normocytic anemia = MCV 80 to 94 fL MCHC >30 g/dL.
What are the causes of increased MCV?
- Pernicious anemia (vit B12 deficiency or folate deficiency).
- Folic acid deficiency.
- Antimetabolite treatment.
- Chronic liver disease.
- Alcoholism.
- Sprue likes steatorrhea, celiac disease, and intestinal resection or fistula.
- Fish tapeworm infestation.
- Carcinoma of the stomach following total gastrectomy.
- Drugs like oral contraceptives, anticonvulsants, anti-tumor agents, and antimicrobial agents.
- Anemia of hypothyroidism.
- Postspenectomy.
- Myelodysplastic syndrome.
What are the causes of decreased MCV?
- Microcytic anemia where MCV <80 fL and MCHC <30 g/dL).
- Iron deficiency anemia.
- Thalassemia.
- Chronic diseases.
- Iron deficiency anemia is usually seen in inadequate iron intake, poor absorption, and chronic blood loss.
- Sideroblastic anemia.
- Anemia of chronic diseases.
- Lead poisoning.
- Disorders of porphyrin synthesis.
What are the causes of normal MCV?
- Normocytic anemia.
- Some hemolytic anemia.
- In some hemoglobinopathies.
- Hypoplastic and aplastic marrow.
Mean corpuscular hemoglobin (MCH):
How will you define MCH?
- This is the mean of the average amount of hemoglobin in red blood cells or the average weight of hemoglobin in absolute units in the RBCs.
- The result gives the average hemoglobin content per RBC in picograms (pg).
- The MCH value is usually higher in newborns and infants because their MCV is higher than that of adults.
What are the Indications of MCH?
- It has limited value in the differential diagnosis of anemia.
- It is instrument calibration.
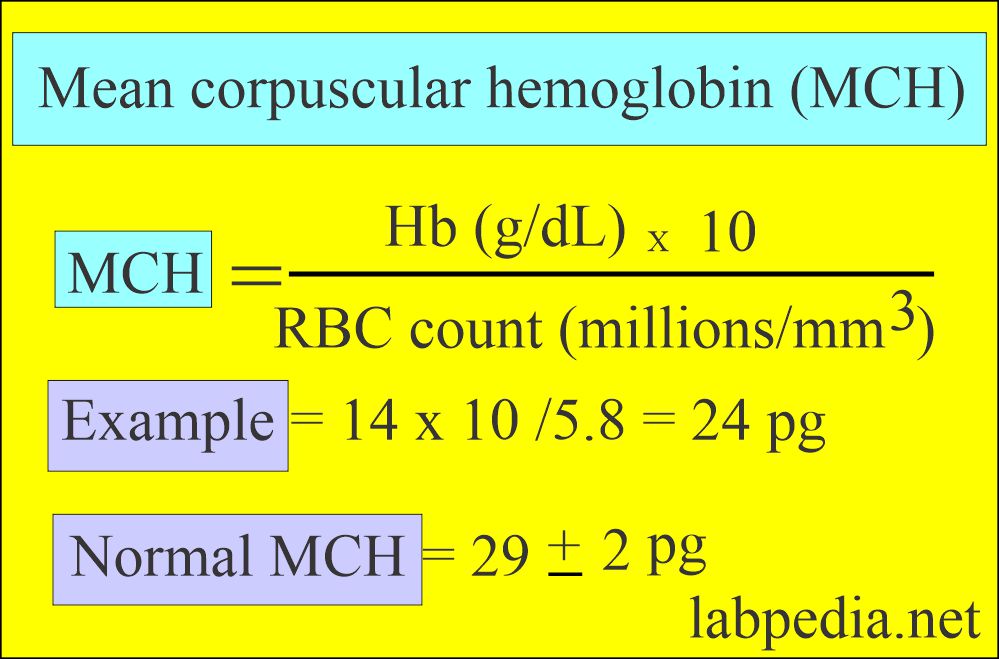
How will you calculate MCH?
- MCH is calculated by multiplying Hb g/dl x 10 and dividing by the RBC count.
- Generally, macrocytes have more hemoglobin, and microcytes have less, so the values resemble those of MCV.
What factors interfere with the estimation of MCH?
- Increased white cell count increases the MCH value.
- Cold agglutinins increase the MCH value.
- Lipemia increases the MCH value.
- High concentrations of heparin increase the MCH value.
- Monoclonal immunoglobulin increases the MCH value.
- In vivo, hemolysis increases the MCH value.
What is the normal MCH value?
- Adult (all ages) = 27 to 31 pg
- Newborn = 32 to 34 pg
What are the causes of increased MCH?
- Macrocytic anemias.
- Newborn.
What are the causes of decreased MCH?
- Microcytic anemias.
- Hypochromic anemia.
Mean corpuscular hemoglobin concentration (MCHC):
How will you define MCHC?
- This is the average concentration or percentage of hemoglobin in each red blood cell.
- It is the ratio of the weight of hemoglobin to the volume of the RBCs.
- MCHC is the most useful for monitoring the treatment of anemia.
What are the indications of the MCHC?
- It is better than MCH to identify hypochromasia.
- Changes in the MCHC appear late in iron deficiency anemia (severe cases).
- It is instrument calibration.
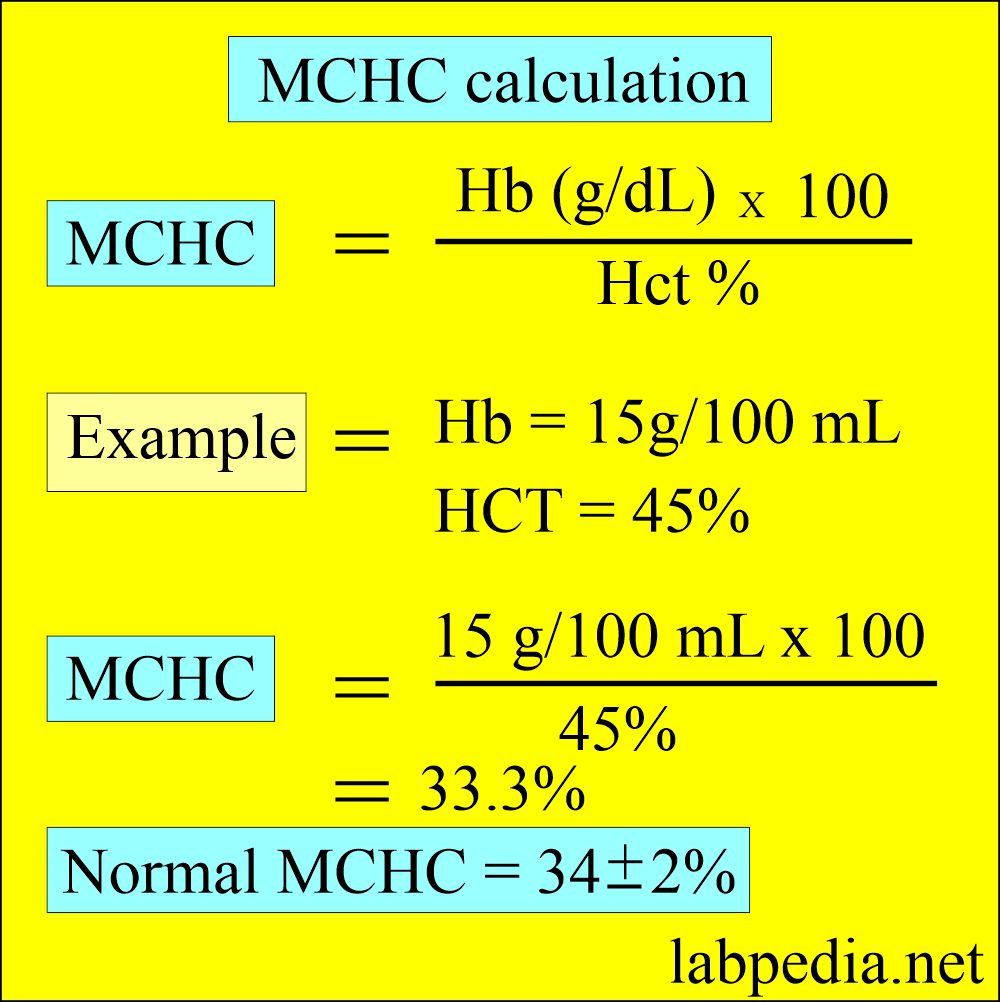
How will you calculate MCHC?
- This is calculated by hemoglobin x 100 divided by hematocrit.
- It is the average amount of Hemoglobin per RBcs (33 to 37 g/dL).
What will interfere with the estimation of MCHC?
- MCHC is decreased in leucocytosis.
- MCHC is increased in hemolysis, such as sickle cell anemia, hereditary spherocytosis, and autoimmune hemolytic anemia.
- Cold agglutinins increase the MCHC.
- Increased concentration of heparin increases the MCHC.
- Rouleaux or RBC agglutination increases the MCHC.
What is normal MCHC?
- Adults of all ages = 32 to 36 g /dl (32 to 36%)
- Newborn = 32 to 33 g /dl (32 to 33%)
How are Red Blood Cells classified based on MCHC?
- Hypochromic When MCHC is decreased, hemoglobin deficiency occurs, e.g., in iron deficiency anemia and thalassemia.
- Normochromic when the values are normal (In hemolytic anemia).
- Hyperchromic when MCHC value is increased, and RBC cannot accommodate more than 37 g/dl (seen in spherocytosis, newborns, and infants).
What are the causes of increased MCHC?
- Spherocytosis.
- Newborns and infants.
What are the causes of decreased MCHC?
- Iron deficiency anemia.
- Thalassemia.
- Microcytic anemia with chronic blood loss.
Red blood cell distribution width (RDW):
How will you define RDW?
- RDW is the quantitative measure of anisocytosis.
- This is the coefficient of the RBC volume distribution.
- This indicates variation in the size of RBC.
- The machine calculates this using MCV and RBC values.
- This is helpful for the diagnosis of hematological disorders and monitoring the response to therapy.
- This is also helpful in distinguishing iron-deficiency anemia (RDW increased) from hemoglobinopathies (RDW normal).
What are the Indications for RDW?
- RDW is used to classify the anemias based on MCv and RDW.
- RDW is more sensitive in microcytic than macrocytic RBC conditions.
- RDW is not helpful in cases without anemia.
How will you calculate RDW?
What is normal RDW?
- Adult = 11.5% to 14.5%
Classify Anemias based on cell size (MCV), and (MCH)?
| Parameter | Interpretation | Diagnosis |
|
|
|
|
|
|
How will you classify anemias based on MCV and MCHC?
| Type of anemia | MCHC% | MCV fL | Causes |
|
32 to 36 | 80 to 100 |
|
|
<32 | <80 |
|
|
32 to 36 | <80 |
|
|
32 to 36 | >100 |
|
Questions and answers:
Question 1: What is the definition of the MCV?
Question 2: What is MCV in microcytic anemia?



It is my choice