Celiac disease and Sprue, Gliadin Antibodies (IgA, IgG), Endomysial Antibodies,
Celiac disease and Sprue
What sample is needed for Gliadin Antibodies IgA and IgG?
- Collect the venous blood to prepare the serum.
- A fasting sample is not necessary.
- An intestinal biopsy may be advised, and it gives characteristic changes.
What are the Indications for Gliadin Antibodies IgA and IgG?
- These antibodies are detected in gluten-sensitive enteropathy.
- This test is done to diagnose Celiac disease and sprue.
- These antibodies are used to monitor the disease.
- In successful treatment with a gluten-free diet, these antibodies will disappear from the serum.
What are the precautions for Gliadin Antibodies?
- Other gastrointestinal diseases, such as colitis, Crohn’s disease, and lactose intolerance, can elevate Gliadin antibody levels.
- Get the list of foods eaten in the last 24 hours.
How will you define Celiac disease/Sprue?
- It is also called Celiac disease, Gluten-sensitivity enteropathy, nontropical sprue, or idiopathic steatorrhea.
- Gluten-induced enteropathy includes Sprue and Celiac disease.
- Both diseases predominantly involved the duodenum and jejunum.
- Celiac disease:
- It is sometimes called non-tropical sprue, celiac sprue, or gluten-sensitive enteropathy.
- Celiac disease is an autoimmune multisystem disease.
- Celiac disease is also called childhood non-tropical sprue.
- A gluten-free diet cures celiac disease.
- The sprue:
- It is an infectious process that is cured by antibiotics.
- Sprue is a broad, nonspecific term that encompasses several conditions characterized by small-intestinal malabsorption.
- Sprue is a nonspecific term for celiac disease and is also known as celiac sprue.
- It also includes tropical sprue and non-celiac gluten sensitivity.
- Tropical sprue is similar to celiac disease, but it occurs in tropical regions with different underlying causes.
- In short, Sprue is a broad term that includes celiac disease and other conditions with similar symptoms and malabsorption.
How will you differentiate between Celeic disease and sprue?
| Parameters | Celiac disease | Sprue |
|
|
|
|
Gluten ingestion | No specific diet relation |
|
Any age (mostly seen in children and adults) |
|
|
|
|
|
Deficiency of :
|
Deficiency of:
|
|
|
Tropical region
|
|
|
|
|
|
|
How will you discuss the epidemiology of Celiac disease?
- It is found predominantly in Europe and, uncommonly, in African Americans.
- It is rare in Asia.
- It is 10-15 times more common in IgA-deficient individuals.
- It is 1% to 3% in patients with type 1 diabetes mellitus.
- There is an association between T-cell lymphoma and juvenile rheumatoid arthritis.
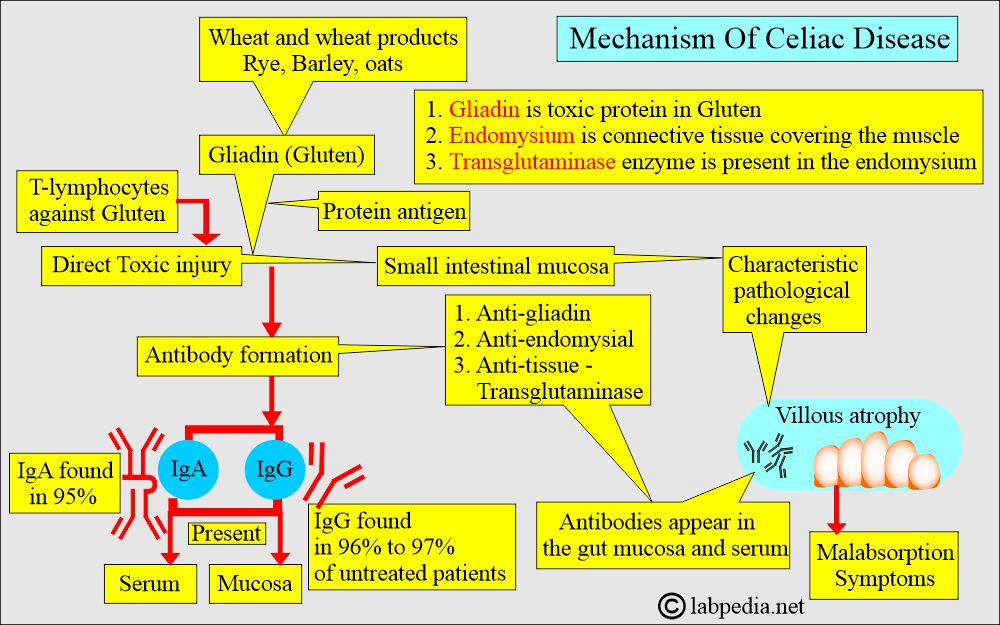
How will you discuss the pathogenesis of Celiac disease and sprue?
- Celiac disease is also called Gluten-sensitive enteropathy, Nontropical sprue, or idiopathic steatorrhea.
- Celiac diseaseia an autoimmune multisystem disorder, mainly present in the GI tract.
- Gliadin is the toxic protein of gluten.
- There is mucosal injury by the complex of gliadin.
- Gliadin is present in wheat, rye, barley, and oats.
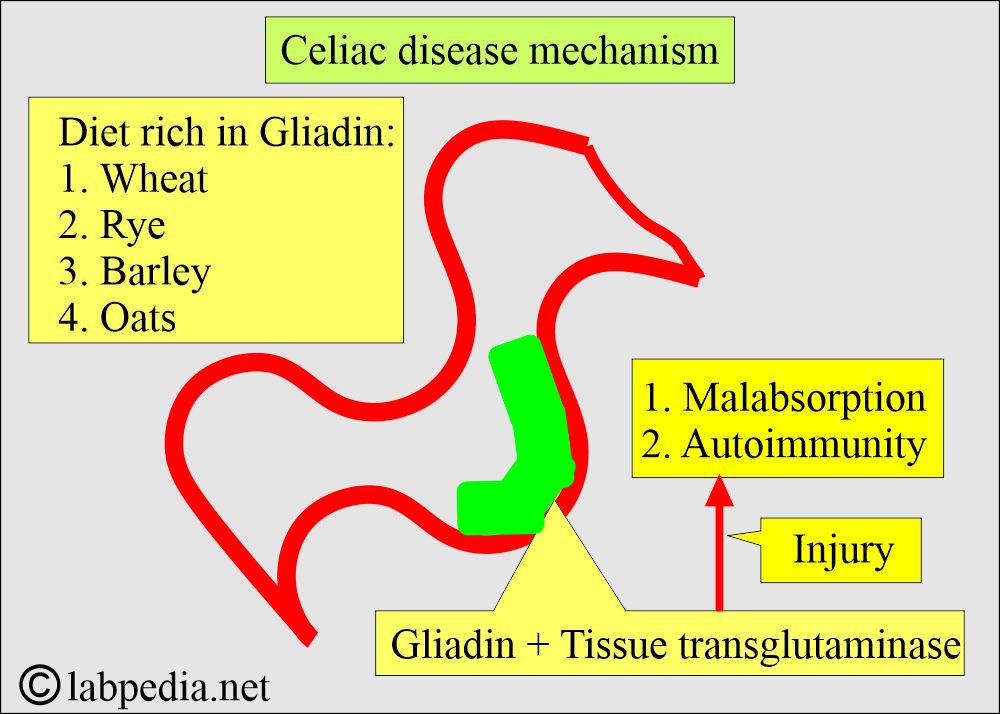
- Gliadin, along with tissue transglutaminase, causes mucosal injury.
- The findings are due to malabsorption and autoimmunity.
- Meanwhile, sprue is a broad term that encompasses malabsorption, as in celiac disease.
What is the mechanism of Celiac disease?
- Gliadin is the complex of gluten and tissue transglutaminase (Gluten + Transglutaminase).
- Tissue transglutaminase is present in the thin connective tissue covering the muscles.
- Gliadin is the toxic protein of gluten.
- Gluten = Gliadin + tissue transglutaminase.
- The small bowel (mainly duodenum and jejunum) tissue Transglutaminase is the auto-antigen.
- The disease’s pathogenesis is believed to involve an interaction between transglutaminase and the gliadin peptide in genetically susceptible individuals.
- In both conditions (celiac disease and sprue), T-lymphocytes mediate an immune reaction against gluten.
- Gluten is found in wheat, rye, barley, and maybe oats.
- There is a genetic predisposition, and it runs in families.
- 10% of the first-degree relatives have this disease.
- There is an association with HLA-DR3 in 90% of patients, and the same is true for dermatitis herpetiformis.
- Another reference states that a genetic component is present on the HLA chromosome 6.
- The major toxic protein of wheat is gliadin.
- There is sensitivity to Gliadin (gluten), which is the protein found in:
- Wheat.
- Wheat products.
- Rye.
- Barley.
- Possible oats.
What antibodies/antigens form in Celiac disease?
- Antibodies to gliadin are toxic agents in celiac disease.
- Patients with celiac disease cannot tolerate the proteins gliadin + gluten in wheat or wheat products.
- Gliadin + gluten are toxic to the small intestinal mucosa and lead to characteristic pathologic changes seen on biopsy.
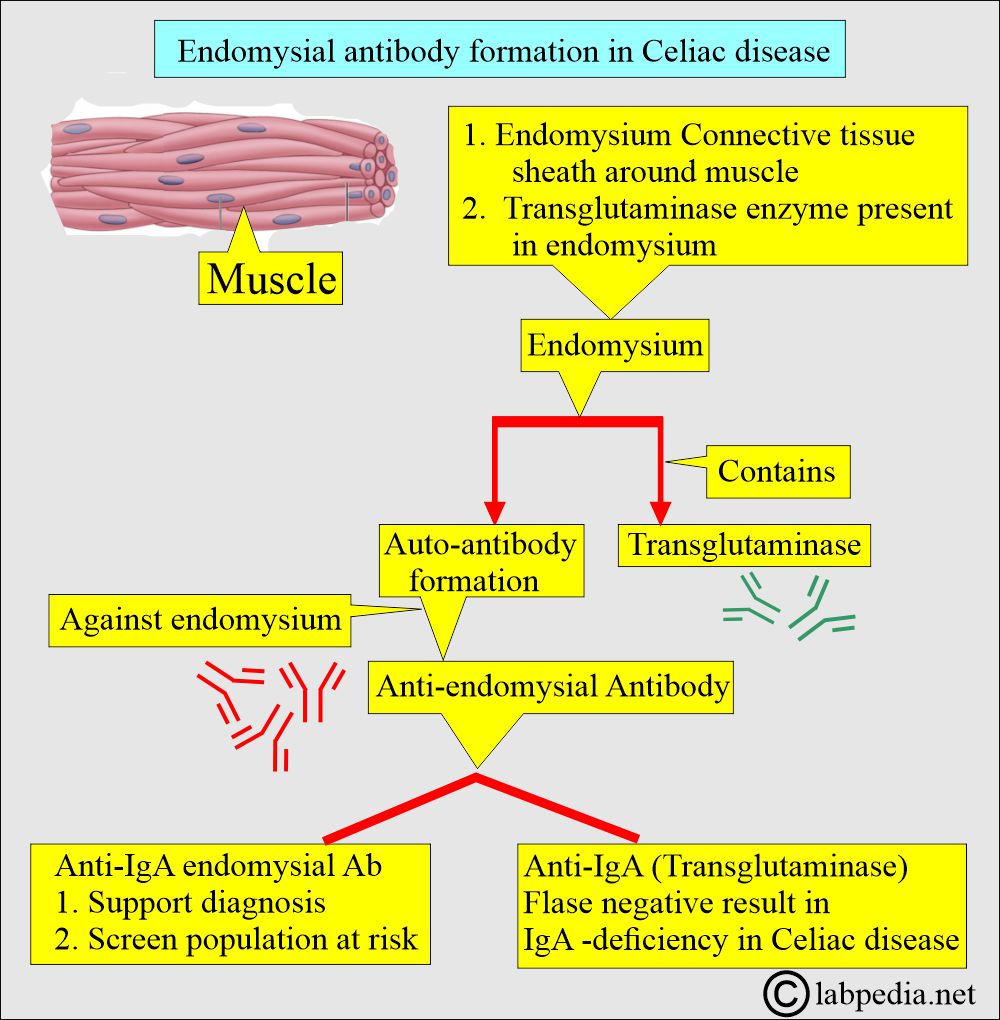
- Endomycelium: It is a thin layer of connective tissue surrounding the muscle.
- These patients develop antibodies against:
- Gliadin = anti-gliadin antibody (IgA and IgG)
- Endomysial = anti-endomysial antibody.
- Tissue = anti-tissue transglutaminase.
- These patients have severe intestinal malabsorption.
- The only treatment for these patients is to avoid wheat and wheat products.
- These antibodies are present in the mucosa and the blood.
- Celiac disease starts in infancy when cereals are given to the baby.
- IgG-antigliadin antibody is more sensitive but less specific than IgA.
- Anti-gliadin antibodies are found in 95% of those with Celiac disease and nontropical sprue.
- Anti-IgG gliadin antibodies are found in 96% to 97% of untreated patients. 80% may have Celiac disease.
- Anti-IgA gliadin antibodies are found in 75% of cases and are 95% specific for Celiac disease.
- Anti-gliadin IgG and IgA antibodies are positive in 45% to 85% of cases of dermatitis herpetiformis.
- False positive cases are seen in ulcerative colitis and Crohn’s disease.
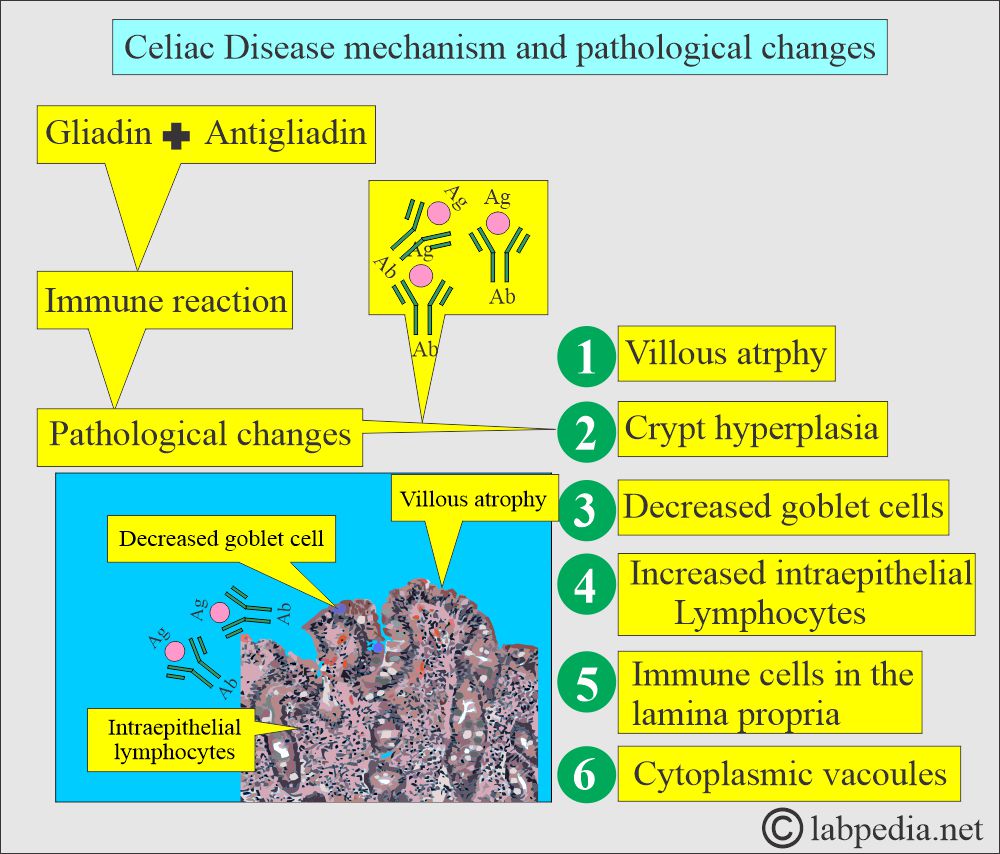
What are the pathological changes in Celiac disease?
There are typical changes on the intestinal (jejunal) biopsy, such as:
- There is villous atrophy.
- Goblet cells are decreased or absent.
- It shows crypt hyperplasia.
- Intestinal epithelial cells show vacuoles.
- The intestinal mucosa first shows blunting of the mucosal villi. There is mild widening and shortening.
- It is followed by flattening and loss of villi.
- There is a lymphocytic infiltrate in the mucosa and submucosa. Also, these cells will infiltrate the lamina propria.
What are the signs and symptoms of Celiac disease?
- Mostly, symptoms appear in children when they start eating cereals.
- The most common presentation is:
- There is easy fatigability.
- There is abdominal bloating and pain.
- There may be vomiting.
- The patient will have chronic diarrhea.
- The stool is foul-smelling, pale, and fatty.
- Sometimes these patients become constipated.
- The stool is hard to flush.
- There are aphthous ulcers.
- The patient will experience weight loss.
- These children are irritable.
- Delay in the growth pattern.
- Sometimes, it is difficult to thrive, and the patient may have osteomalacia.
- There is a strong association with other autoimmune diseases like type 1 diabetes mellitus and autoimmune thyroid diseases.
What are the complications of Celiac disease?
- There is anemia.
- 15% to 20% of patients develop intestinal lymphoma or adenocarcinoma.
- There is an increased incidence of gastric and esophageal carcinoma.
- There may be neuropathy.
- These patients may have hyposplenism.
What is the normal Gliadin-antibody?
- Values are given for the child of age >2 years:
- Negative = <25 U/L .
- Weak positive = 25 to 50 U/L.
- Positive = >50 U/L.
Source 6
- Gliadin IgA/IgG = 0 to 2 years = <20 EU.
- 0 to 3 years and older = <25 EU.
- Endomysial IgA = all ages = negative.
- Tissue transglutaminase IgA = all ages = <20 EU.
How will you diagnose celiac disease?
- An elevated level of anti-gliadin and anti-endomysial antibodies.
- IgA and IgG antibody sensitivity are 90% for the active, untreated disease. When both antibodies are done, the specificity is also 90%.
- These antibodies will detect the following diseases:
- Celiac disease will have 100% IgA endomysial antibodies.
- Celiac sprue.
- Anti-IgA endomysial antibody:
- It is the antibody test of choice for diagnosing celiac disease.
- This antibody can be used to screen the population.
- Anti-gliadin IgA antibody:
- This antibody disappears after 3 to 6 months of gluten abstinence.
- It may be used to monitor the diet restriction.
- It is the best marker for children under <3 years old.
- Gliadin is a component of gluten.
- Anti-IgA transglutaminase antibody:
- False results may occur in IgA deficiency.
- More reproducible than anti-IgA endomysial antibodies.
- Dermatitis herpetiformis 70% shows IgA endomysial antibodies.
- Intestinal (jejunum) biopsy shows typical changes in villous atrophy.
- On jejunal biopsy, we will see villous atrophy.
- Increased intra-epithelial lymphocytic infiltrate.
- There is hyperplasia of the crypts.
- These changes may reverse on a gluten-free diet. This will not occur in the sprue.
- In Celiac disease, anemia may be macrocytic or hypochromic microcytic.
What are the serological tests for Celiac disease?
| Antibody | Specificity | Sensitivity |
|
95% | 75% to 95% |
|
>99% | 80% to 100% |
|
|
>95% |
What are the diagnostic criteria for the Celiac disease?
- Provisional diagnosis:
- Positive serological (anti-gliadin antibody) test.
- Typical pathological findings on biopsy of the small intestine.
- The confirmatory test is:
- When a gluten-free diet is given, patients become symptom-free.
- Serological tests fall within the normal range or are negative.
- The pathological changes will improve or disappear if a biopsy is done.
How will you treat Celiac disease?
- Start a permanently gluten-free diet.
- Avoid wheat, barley, rye, and oats.
- Another reference excludes oats, which are allowed in the list of edible foods. Be sure there is no mixing of wheat, barley, or rye.
- Or any food containing them, like bread, cake, and pies.
- Rice, soya, potatoes, maize, jam, and sugar are allowed.
- Gluten-free flour, bread, and pasta are available.
- Try steroids if diet therapy is not helpful.
Questions and answers:
Question 1: What are the false positive conditions for Anti-gliadin antibodies?
Question 2: What is the result of Celiac disease?