Anti-GBM antibody (Anti-Glomerular basement membrane antibody), Good Pasture Syndrome
Anti-GBM antibody
What sample is needed for the Anti-GBM antibody?
- This test is done on the venous blood to get the serum.
- The patient needs to fast for 8 hours.
- Another sample is a tissue biopsy of the kidney and lung tissue. It is used for microscopic evaluation.
What are the Indications for anti-GBM antibody?
- To diagnose autoimmune-induced glomerulonephritis.
- To differentiate from the other type of glomerulonephritis.
- To diagnose Goodpasture’s syndrome.
What are the precautions for the Anti-GBM antibody?
- Drugs like antibiotics may decrease the test result.
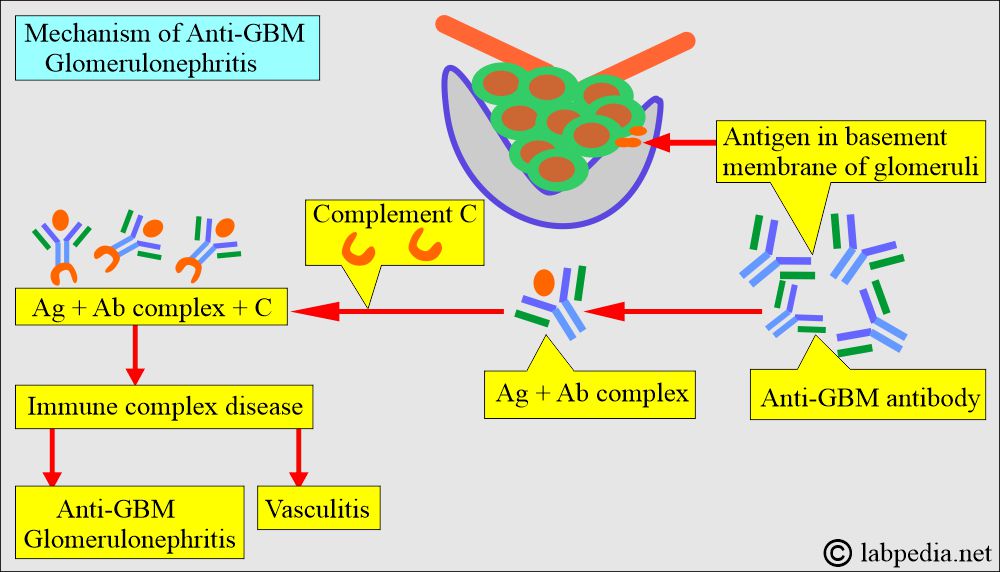
How will you discuss the pathophysiology of Anti-GBM glomerulonephritis?
- This is an autoimmune phenomenon.
- About 5% of glomerulonephritis is of the Anti-GBM type.
- Some autoantibodies react with the basement membrane of the renal glomeruli capillaries.
- These autoantibodies react with small blood vessels of the kidney and lung.
- These autoantibodies react with pulmonary alveoli.
- When these antibodies react only with the glomeruli’s basement, they produce anti-GBM glomerulonephritis.
- In Goodpasture’s syndrome, antibodies against the glomerular basement membrane circulate. These antibodies also react against the lung alveoli.
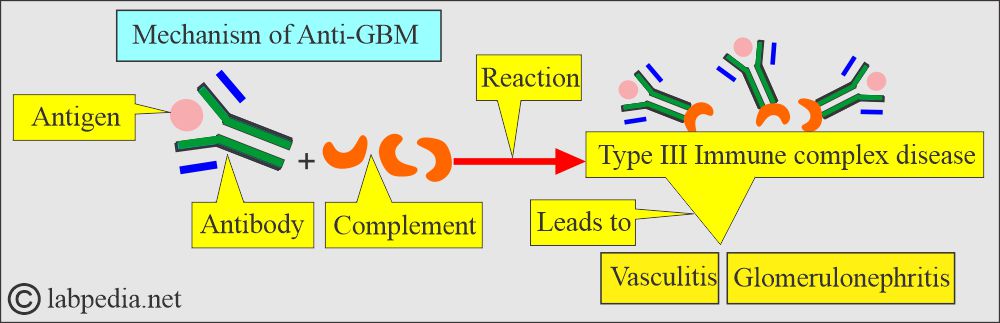
What is the mechanism of tissue damage?
- It is a type III hypersensitivity reaction where immune complexes activate the complement system.
- Immune complexes give rise to:
- Glomerulonephritis leads to hematuria.
- Pulmonary hemorrhage leads to hemoptysis.
- Positive autoantibodies against basement membranes.
- This hypersensitivity reaction is complement-mediated.
- The damage is due to the deposition of immune complexes.
Goodpasture syndrome:
How will you define Goodpasture syndrome?
- It is an autoimmune disease characterized by the following:
-
- When both kidneys and lungs are involved.
- Hematuria.
- Hemoptysis (pulmonary hemorrhage).
- Antibodies react to the kidneys and lungs’ basement membrane (antigen).
- Both kidneys and lungs are involved in 60% to 70 % of cases (Goodpasture syndrome).
- 20% to 40 % of the cases show only involvement of the kidneys, only then called anti-GBM glomerulonephritis.
- The patient will have a bloody cough when the lungs are involved.
How will you diagnose Anti-GBM glomerulonephritis and Goodpasture syndrome?
- The serum method is easier, faster, and more reliable for patients with a difficult or contraindicated biopsy.
- Blood by enzyme immunoassay (EIA):
- Negative = <20 units
- Borderline = 20 to 100 units
- Positive = >100 units
- The high anti-GBM titer is suggestive of the following:
- Goodpasture’s syndrome.
- Lupus erythematosus.
- Anti-GBM nephritis.
- A lung or renal biopsy demonstrates these antibodies using an immunohistochemical technique.
What is the normal anti-GMB antibody?
Source 2
Blood (EIA enzymatic immunoassay):
- Negative = <20 units.
- Borderline = 20 to 100 units.
- Positive = >100 units.
Tissue biopsy:
- Negative = No immunofluorescence was seen on renal or lung biopsy.
Source 4
- Negative = <5 EU/mL by ELISA
- Borderline = 5.1 to 20.0 EU/mL
- Positive = 20.1 to 400 EU/mL
- A negative result does not rule out Goodpasture’s syndrome.
Where will you see the Anti-GBM antibody?
- Autoimmune glomerulonephritis.
- Goodpasture’s syndrome.
- Tubulointerstitial nephritis.
- Some patients have lupus nephritis.
Questions and answers:
Question 1: What is the criteria for Goodpasture syndrome?
Question 2: What is the significance of anti-GBM antibody?