Gram Stain
What sample is needed for a Gram Stain?
- The Gram stain can be performed on sputum, pus, tissue, and urine.
- The sample can be obtained from the infected ulcer or wound.
- The CSF may be stained.
What are the indications for a Gram stain?
- The Gram stain differentiates between Gram-positive and Gram-negative organisms.
- To diagnose the presence of bacteria in sputum, pus, or any other tissue or fluid.
- To diagnose bacterial meningitis.
- It can stain yeast, and this needs to be reported.
What is the history of the Gram stain?
- Bacteria are colorless and usually invisible under light microscopy, so a stain was developed to visualize them.
- The name comes from its inventor, Hans Christian Gram. He published a Gram stain method in 1884.
- He was searching for the organism and was diagnosed with pneumonia.
- This is a special stain for diagnosing Gram-positive or Gram-negative organisms in various samples, such as sputum, pus, and urine.
- Bacteria that absorb crystal violet and retain it appear blue; these are called Gram-positive organisms.
- If the crystal violet is washed off with alcohol, it will absorb the counterstain safranin, which stains gram-negative organisms.
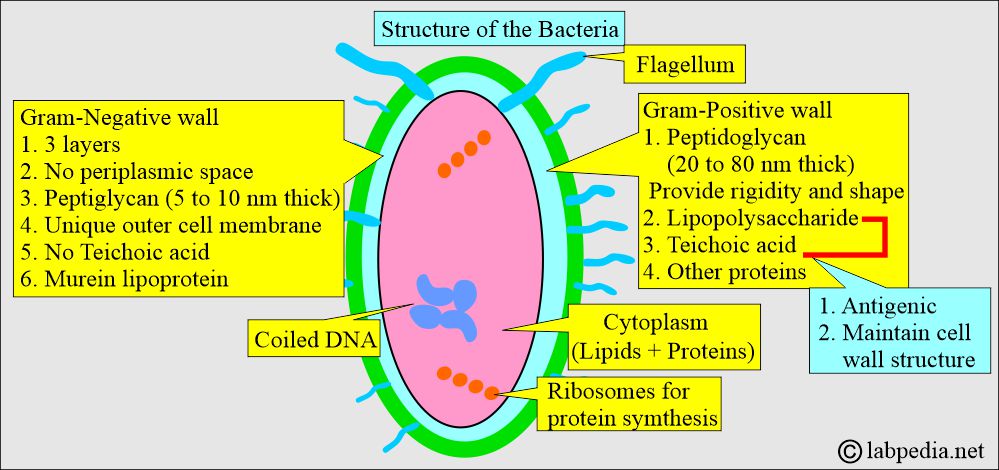
What is the structure of the bacteria?
- Bacteria are prokaryotes (single-cell organisms).
- The layer outside the cytoplasm is called the peptidoglycan layer and is present in both Gram-positive and Gram-negative bacteria.
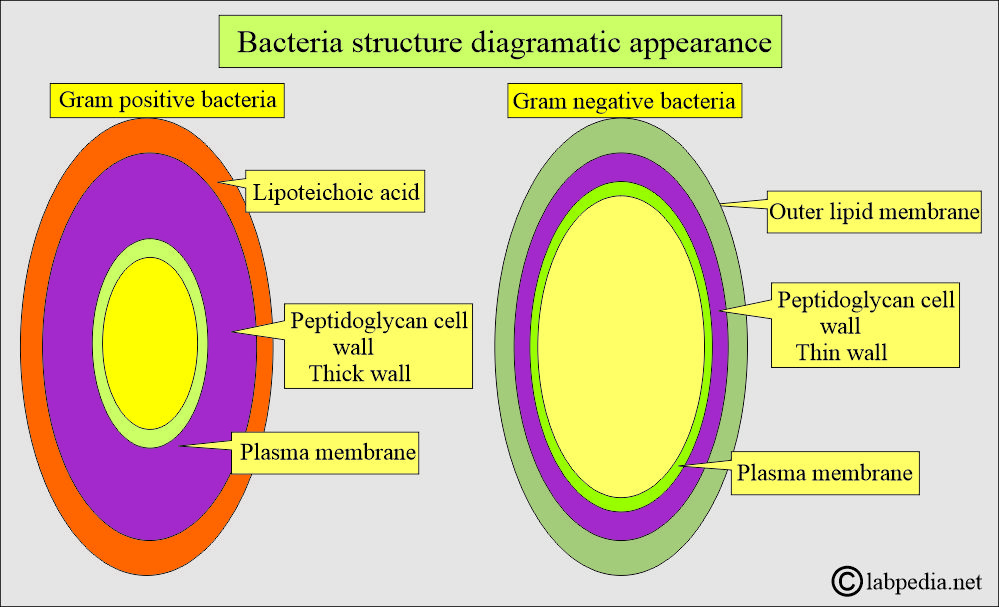
- Gram-positive bacteria have a thick wall and extensive cross-linking of the amino acid chains. In contrast, gram-negative bacteria have a very thin wall and a simple cross-linking pattern.
- Bacteria consist of circular DNA molecules (Continuous coding of the gene).
- DNA is tightly coiled.
- Only ribosomes are seen, which are needed for protein synthesis.
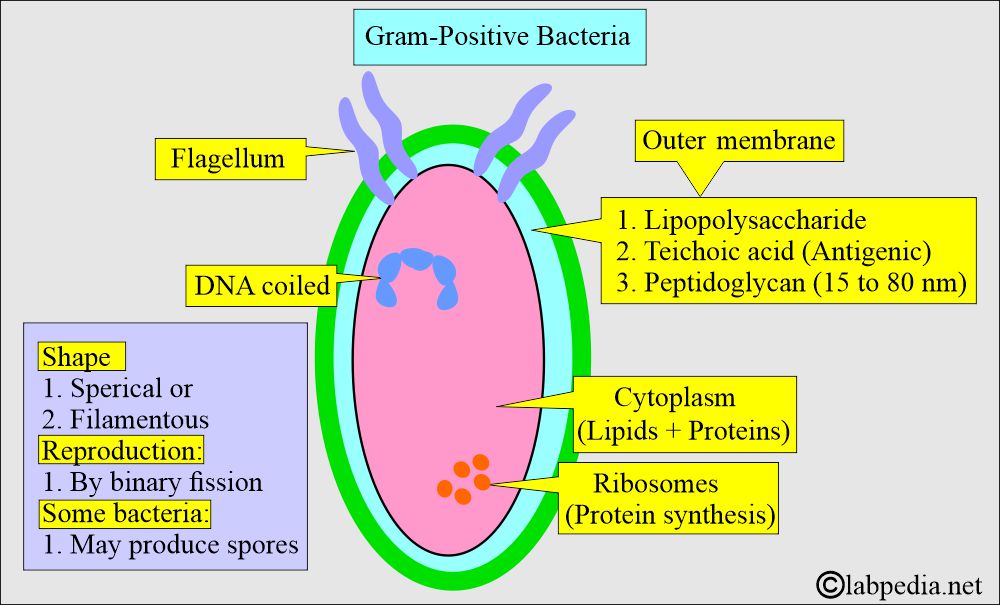
- Gram-positive organisms are hydrophilic, and this property prevents bacteria in the intestine from being affected by bile.
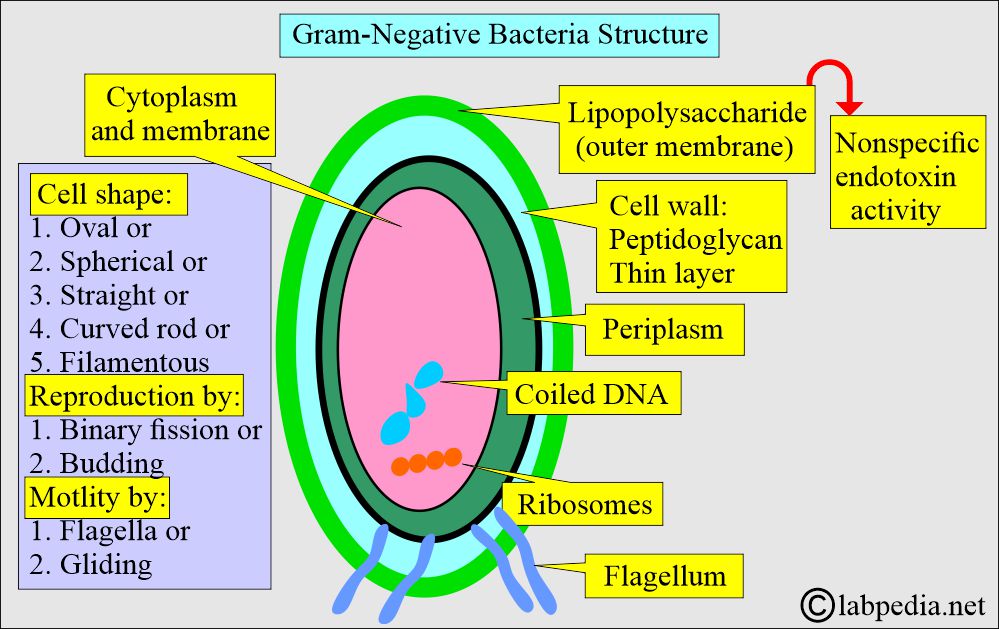
- Gram-negative bacteria’s outer cell walls are also hydrophilic, but the lipid component molecules give hydrophobic properties.
How will you classify the bacteria?
- Gram-positive = Blue.
- Gram-negative = Red.
- The gram-negative bacterial wall consists of three layers.
- Gram-positive bacteria consist of two layers.
How will you differentiate Gram-positive and Gram-negative bacteria?
| Characteristic features | Gram-positive | Gram-negative |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
How will you do Gram staining?
What solutions are needed for the Gram stain?
- Crytal violet = 0.5% in distle water.
- Gram’s iodine:
- iodine = 1 gram
- Potassium iodide = 2 grams
- Distle water = 300 mL
- Ethyl alcohol 75%.
- Dilute carbol fuschsin:
- Zeihl-Nelsen carbolfichsin = one part
- Distle water = 9 parts
- Acetone:
- Acetone, 1 part with 2 parts ethyl alcohol, is a much more rapid decolorizer than 70% ethyl alcohol.
- Neutral red:
- Neutral red 1 gram, 1% acetic acid 2 mL, and distilled water 1000 mL, may be used as a counterstain.
- It is useful for staining intracellular organisms and does not mask weakly gram-positive organisms.
- Safranin:
- Safranin 0.5% in distle wateris another counterstain.
- But it has no obvious advantages.
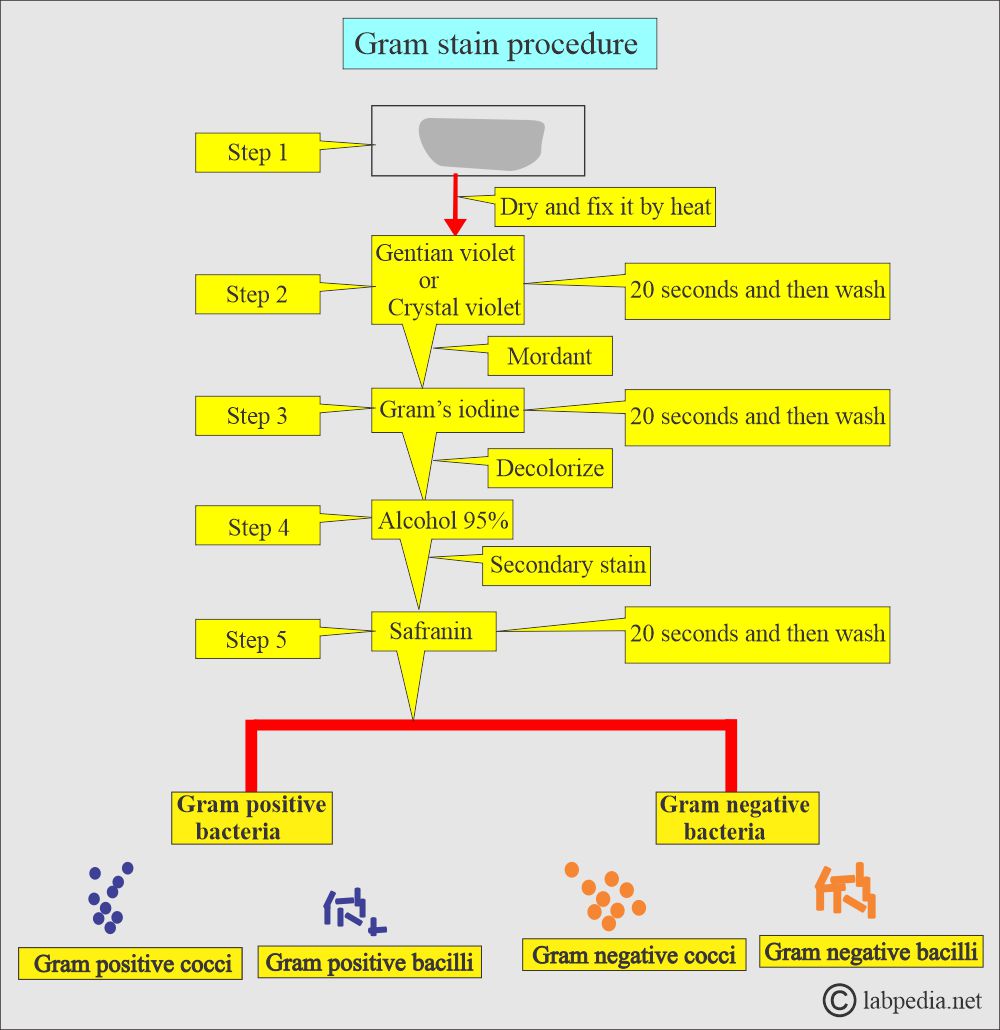
What are the steps in the Gram stain?
- Fix the slide by heating.
- Primary stain: Stain the slide smear with gentian violet or crystal violet. It will penetrate the cell membrane.
- Mordant: Wash the violet stain and flood the smear with the Iodine solution. This acts as a mordant and forms a complex with Crystal violet.
- Decolorizer: Wash off the smear and flood it with alcohol (95 %) or an Acetone-alcohol mixture.
- This will remove the outer membrane of Gram-negative bacteria, after which the complex will be washed off.
- Gram-positive bacteria’s cell membrane remains intact, and the stain will not be washed off after alcohol treatment.
- Decolorization with acetone or alcohol will lead to the following:
- Gram-positive bacteria block dye extraction (still unclear).
- This step will decolorize gram-negative bacteria and not gram-positive bacteria.
- Secondary stain: Counterstain the smear with safranin O, a red dye, or carbolfuchsin.
- Counterstaining with dilute carbol fuchsin is done for one minute
- The counterstain cannot enter Gram-positive bacteria, so they appear purple.
- In gram-negative bacteria, safranin can enter and give a pink color.
- Rinse in water and dry.
How will you report the results of the Gram stain?
- Gram-positive bacteria are blue-purple.
- Gram-negative bacteria are pink magenta.
- Coagulase-positive bacteria are Staphylococcus aureus.
- Coagulase-negative bacteria are S. epidermidis, S. saprophyticus, and S. hemolyticus.
How will you give some examples of Gram-stained bacteria?
| Type of microorganism | Morphology in Gram stain |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
How will we classify bacteria based on the Gram stain?
| Bacteria | Gram-positive | Gram-negative |
|
|
|
|
|
|
What are the examples of Bacterial Infections?
- Gram-positive cocci infections:
- Staphylococcus aureus can cause skin infections.
- Toxic shock syndrome.
- Gram-negative cocci infections:
- N. meningitidis causes meningitis.
- N. gonorrhoeae causes gonorrhea.
- Gram-negative bacilli infections:
- E.coli causes urinary tract infection.
- Gram-positive bacilli infections:
- B. anthracis causes skin infection and pneumonia.
- Listeria monocytogenes may cause food-borne infection.
- Viruses do not stain with the Gram stain.
Questions and answers:
Question 1: Who was the inventor of the Gram stain?
Question 2: What is the role of safranin counterstaining for gram-negative bacteria?